Table of Contents
Introduction
74% of hospitals are already using some form of automated revenue cycle management software.
But there are still gaps in complete revenue cycle management improvement. Most practices still manage registrations, insurance checks, and payments manually.
This leads to lost time and missed revenue every day.
Read this guide to learn how automation can close critical RCM gaps. Here’s what this blog covers:
- What is revenue cycle management (RCM) really means
- Revenue cycle management hospitals face common challenges
- How to improve revenue cycle management and run a more efficient operation
- Revenue cycle management benefits of automation
- How digital solutions like CERTIFY Health can help you streamline payments and collect revenue faster
Understanding Revenue Cycle Management
Define Revenue Cycle Management in Healthcare
Revenue cycle management in healthcare is the process hospitals and healthcare providers use to manage the financial side of patient care, from scheduling and insurance verification to billing and payment collection.
The healthcare revenue cycle management process ensures services are documented correctly, claims are submitted on time, and payments are collected accurately, helping organizations maintain steady cash flow and reduce revenue loss.
Healthcare Revenue Cycle Management Process

TL; DR:
Healthcare Revenue Cycle Management Process
- Patient Registration
Collectaccurate patient and insurance details to prevent billing errors. - Insurance Verification
Confirm coverage early to reduce claim denials and payment delays. - Charge Entry & Claim Filing
Submitaccurate codes and claims to ensure faster reimbursement. - Claims Review & Payment Resolution
Process claims efficiently tomaintain steady cash flow. - Denial Prevention & Appeals Management
Fix and resubmit denied claims to recover lost revenue. - Reporting & Financial Analysis
Use data insights to improve performance and strengthen revenue.
A strong RCM process ensures providers capture revenue accurately, reduce denials, and maintain steady cash flow.
Steps include:
1. Patient Registration
This step begins when a patient schedules an appointment or arrives for care. Staff collect and verify essential details such as the patient’s name, contact information, demographics, and insurance coverage.
Why it matters:
Accurate registration prevents billing errors, reduces claim rework, and improves first-pass claim acceptance, an important part of effective revenue cycle management.
2. Insurance Verification
The insurance eligibility verification process confirms whether a patient’s plan is active and what services are covered. It also identifies deductibles, co-pays, and prior authorization requirements.
Why it matters:
Verifying coverage upfront helps prevent denied claims and ensures patients understand their financial responsibility before treatment begins. This is a key revenue cycle management best practice.
3. Charge Entry & Claim Filing
After services are delivered, providers document procedures and assign the correct medical codes. These codes are converted into billable charges and submitted to payers as claims.
Why it matters:
Accurate coding and timely claim submission reduce denials, speed reimbursement, and protect revenue integrity, crucial for revenue and payment cycle management.
4. Claims Review & Payment Resolution
Insurance companies review submitted claims to confirm medical necessity and policy compliance. Approved claims result in reimbursement to the provider based on contracted rates.
Why it matters:
Efficient claims processing ensures predictable revenue cycles and minimizes payment delays. This is part of techniques and tools for improving healthcare revenue cycle management.
5. Denial Prevention & Appeals Management
Denied or rejected claims are reviewed to identify the root cause. Staff correct errors, provide additional documentation, and resubmit claims or file appeals when necessary.
Why it matters:
Proactive denial management reduces revenue leakage and improves overall collection rates; another revenue cycle management best practice.
6. Reporting & Financial Analysis
Revenue cycle leaders use reporting and analytics to monitor key financial metrics such as claim status, payment trends, and outstanding balances.
Why it matters:
Data-driven insights help organizations identify inefficiencies, optimize workflows, and strengthen financial performance. This aligns with how a healthcare organization can improve its revenue cycle management.
An effective revenue cycle management system not only maintains a steady cash flow for healthcare practices but also reduces claim denials and administrative burdens for staff, leading to improving revenue cycle management overall.
Pro Tip:
Implementing modern revenue cycle management best practices isn’t just about efficiency; it’s about protecting your revenue and staying financially stable.
With automation from CERTIFY Health, you can streamline the entire revenue cycle, from patient registration and eligibility verification to clean claims submission and denial prevention, without adding more work for your staff.
The result:
- Fewer claim denials
- Faster collections
- Less administrative burden
- More predictable cash flow
The Challenges of Revenue Cycle Management
TL; DR:
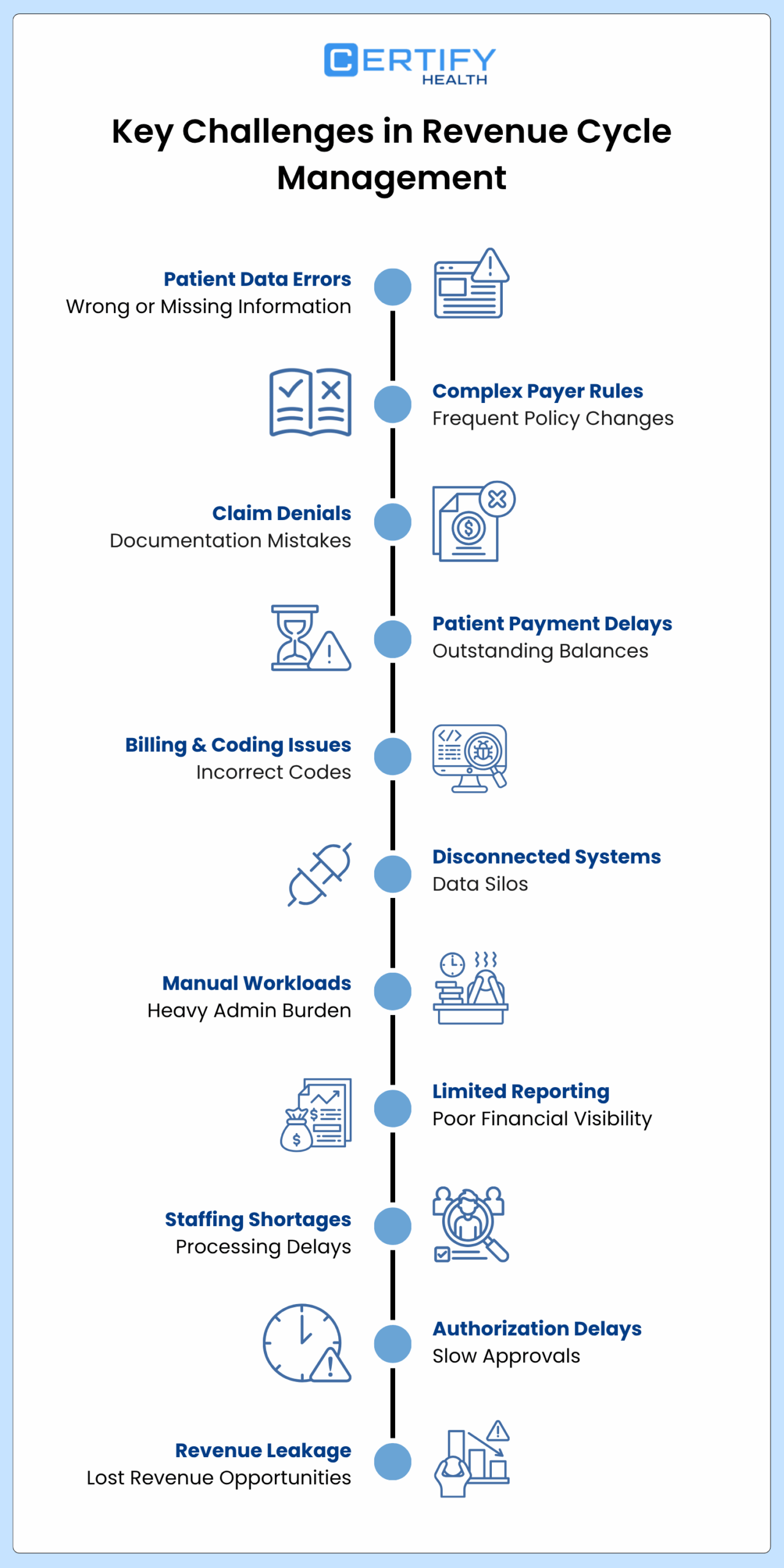
Key Challenges in Revenue Cycle Management
- Patient Data Errors
Incorrect information leads to claim delays and denials. - Complex Payer Rules
Changing policies increase compliance risks and slow payments. - Claim Denials
Errors in coding or documentation reduce revenue. - Patient Payment Delays
Unpaid balances increase accounts receivable. - Billing and Coding Issues
Mistakes cause rejections and reimbursement delays. - Disconnected Systems
Poor integration creates inefficiencies and errors. - Manual Workloads
Manual tasks increase staff burden and slow collections. - Limited Reporting
Lack of visibility weakens financial control. - Staffing Shortages
Fewer staff slow processing and increase errors. - Authorization Delays
Slow approvalspostpone care and payments. - Revenue Leakage
Missed charges and follow-ups reduce profitability.
Revenue cycle management challenges often stem from operational inefficiencies, staffing limitations, and increasing financial pressure from payers and patients. These issues lead to delayed payments, higher denial rates, and reduced cash flow for healthcare organizations.
1. Incomplete or Incorrect Patient Information
Errors in patient names, insurance details, or demographic data can disrupt the RCM process from the very beginning.
Impact: Claims may be delayed or denied, increasing rework and slowing reimbursement.
2. Complex Insurance Policies and Regulations
Healthcare organizations must navigate constantly changing payer rules, coverage policies, and compliance requirements.
Impact: Regulatory errors can lead to payment delays, financial penalties, and lost revenue.
3. Claim Denials and Rejections
Claims are frequently denied when documentation is incomplete, coding is inaccurate, or payer requirements are not met.
Impact: High denial rates increase administrative workload, delay payments, and reduce overall revenue.
4. Rising Patient Financial Responsibility
Patients are responsible for a growing share of healthcare costs, including deductibles and co-pays.
Impact: Delayed or uncollected patient payments reduce cash flow and increase accounts receivable.
5. Inefficient Billing and Coding Processes
Incorrect diagnosis or procedure codes can occur when staff lack proper training or documentation is incomplete.
Impact: Billing mistakes lead to claim rejections, payment delays, and reduced financial performance.
6. Lack of Integration Between Systems
Disconnected systems prevent smooth data flow across the revenue and payment cycle management.
Impact: Fragmented workflows increase errors, slow operations, and reduce overall efficiency.
7. Manual Workflows and Administrative Burden
Manual tasks consume significant staff time and increase errors.
Impact: Administrative burden contributes to staff burnout, higher error rates, and slower revenue collection.
8. Limited Financial Visibility and Reporting
Without real-time reporting tools, healthcare leaders may struggle to monitor revenue trends.
Impact: Poor visibility into performance can lead to missed revenue opportunities and weak financial control.
9. Staffing Shortages and Skill Gaps
Limited staffing slows claim processing and increases errors.
Impact: Workforce shortages delay reimbursement and reduce efficiency in revenue cycle management hospitals.
10. Prior Authorization Delays
Obtaining prior authorization from insurers can be time-consuming.
Impact: Authorization delays postpone treatment, disrupt scheduling, and slow revenue flow.
11. Revenue Leakage
Revenue leakage occurs when charges are missed or denied claims are not followed up.
Impact: Unresolved revenue gaps reduce profitability and weaken financial stability.
These challenges affect profitability and patient satisfaction. When patients experience confusion about their medical bills or struggle to pay, it impacts the practice’s overall trust and efficiency.
How To Improve Revenue Cycle Management Using Automation to Streamline Payments

TL;DR:
How to Improve Revenue Cycle Management Using Automation
- Automate Verification & Prior Authorization
Confirm coverage early to prevent denials and speed approvals. - Automate Claim Submission
Submit clean claims faster to reduce rejections and delays. - Automate Payment Posting (ERA)
Auto-post payments to improve accuracy and reconciliation. - Integrate Systems
Connect EHR, billing, and payments toeliminate duplicate work. - Use Claim Validation Tools
Catch errors before submission to lower denial rates. - Send Automated Billing Reminders
Notify patients regularly to improve on-time payments. - Offer Digital Payment Options
Provide online and flexible payment methods to accelerate collections. - Train Staff on Automation Tools
Ensure teams use systems correctly to boost productivity. - Use Data Analytics
Track KPIs to identify issues and improve cash flow.
You don’t need more tools or staff to fix challenges with revenge cycle management.
Revenue cycle management best practices require implementing CERTIFY Health’s revenue cycle management automation tool.
It automates repetitive administrative tasks and the RCM process, improving staff efficiency and data flow, preventing errors, improving collections, and boosting patient satisfaction.
1. Start with Verification & Prior Authorization
If your staff does not properly verify patient insurance eligibility and prior authorization requests, your claims may never be paid.
CERTIFY Health’s Patient-side Revenue Tool automates insurance verification and prior authorization, helping improve revenue cycle management.
Once patient insurance card details are updated, the system automatically verifies eligibility and submits authorization requests.
The results?
Verified details before care begins, fewer claim denials, and faster approvals.
2. Automate Claim Submission Process
Manual claim submission is risky.
CERTIFY Health’s Billing & Claims Tool generates and submits clean claims with built-in validation checks.
The result?
Faster submissions, fewer rejections, and more predictable cash flow, an example of automated revenue cycle management improving efficiency.
3. Automate Payment Posting with ERA
Manual payment posting is not only tiresome but highly prone to data entry mistakes or errors.
Small mistakes can have a ripple effect, leading to billing errors and slower financial reconciliation.
Electronic Remittance Advice (ERA) automatically posts payments, reducing errors.
CERTIFY Health Automates Back-office Workflows, improve reconciliation and help finance teams to close books faster and maintain accurate financial records, supporting effective revenue cycle management.
4. Use Integrated Systems to Eliminate Data Silos
Many healthcare organizations still rely on separate systems for scheduling, billing, and patient records. When systems do not connect, staff must re-enter the same data multiple times.
An integrated RCM platform connects these workflows into a single system. Information flows automatically between departments without manual updates.
CERTIFY Health’s integrations connect EHR, billing, and financial systems, reducing duplication and errors, allowing organizations to improve revenue cycle management.
5. Prevent Claim Denials with Automated Validation Tools
Denied claims are one of the biggest causes of revenue delays. Errors often happen when required information is missing, or payer rules are not followed.
Automated claim validation ensures compliance and accuracy, reducing denials and delays, an essential technique and tool for improving healthcare revenue cycle management.
CERTIFY Health’s automated claim validation flags errors and missing information before submission, ensuring claims meet payer requirements from the start.
The impact?
Lower denial rates, faster payments, and stronger revenue protection.
6. Improve Patient Communication with Automated Billing Reminders
Patients are more likely to pay on time when they understand their bills and receive reminders. Without follow-ups, balances can remain unpaid for long periods.
Automated billing notifications help patients pay on time, enhancing revenue cycle management benefits.
CERTIFY Health automates billing notifications, digital statements, and payment reminders via email or text.
It also sends dunning notices and overdue reminders to patients, helping ensure follow-ups happen consistently without adding extra work for your staff.
7. Offer Flexible Digital Payment Options
Modern patients expect simple and convenient ways to pay their medical bills. Limited payment options can delay collections and increase outstanding balances.
Digital payment tools allow patients to pay online, set up payment plans, or use contactless methods from their phone or computer.
CERTIFY Health’s CERTIFY Pay allows patients to pay online or via contactless methods, helping streamline payments and reduce outstanding balances.
By giving patients multiple ways to pay, your practice removes friction from the payment process and makes it easier to collect on time.
8. Train Staff to Use Automation Effectively
Technology works best when staff know how to use it confidently.
Without proper training, teams may rely on manual work even when automation is available.
Providing regular training helps employees understand workflows, use tools correctly, and solve problems quickly. Proper staff training maximizes the benefits of automated revenue cycle management.
Impact: Better productivity, fewer errors, and smoother operations.
9. Use Data Analytics to Monitor Revenue Performance
Healthcare leaders need clear visibility into how money moves through the revenue cycle. Without KPI data, it is difficult to identify problems or measure progress.
CERTIFY Health’s analytics dashboard tracks KPIs like claim denial rates and payment trends, helping organizations focus on revenue cycle management improvement and informed decision-making.
Consolidating this data in one place, practices can quickly identify inefficiencies, spot revenue leakage, and make informed decisions to improve cash flow.
Impact: Stronger financial planning and continuous process improvement.
Conclusion
Improving Revenue Cycle Management (RCM) goes beyond billing; it strives to make payments easy and quick both for patients and providers.
Automating key processes, providing flexible payment options, and employing advanced RCM helps healthcare practices improve collections, reduce claim denials, and reap more financial benefits.
CERTIFY Health’s revenue cycle management software simplifies payment collection and improves efficiency with its comprehensive front-to-back-end RCM solutions.
Now is the time to rethink your RCM strategy and embrace digital solutions for a more efficient, profitable, and patient-friendly practice.
Tap the Link to Book a Demo with CERTIFY Health or Explore Top 10 Revenue Cycle Management Software
FAQs
What is RCM in healthcare?
RCM, or Revenue Cycle Management, is the process healthcare organizations use to manage billing, insurance claims, and payment collection from patient scheduling to final payment. It ensures services are documented, billed correctly, and reimbursed on time.
What is the goal of RCM?
The goal of RCM is to ensure healthcare providers are paid accurately and on time. It improves cash flow, reduces billing errors, minimizes claim denials, and keeps financial operations running smoothly.
How can a healthcare organization improve its revenue cycle management?
Revenue cycle management can be improved by verifying patient information accurately, submitting clean claims quickly, reducing claim denials, following up on unpaid balances, and using automation tools to streamline billing and payment processes.
What is KPI in revenue cycle?
A KPI, or Key Performance Indicator, in revenue cycle management is a measurable metric used to evaluate financial performance. Common KPIs include days in accounts receivable, claim denial rate, collection rate, and payment turnaround time.
What does payment posting mean in RCM?
Payment posting in Revenue Cycle Management (RCM) is the process of recording payments received from insurance companies or patients and applying them to the correct accounts. This ensures accurate financial records and helps identify underpayments or billing errors.






















