Table of Contents
Dermatology hospitals face soaring demand but crippling inefficiencies: 30% no-shows drain slots, 14-20% claim denials tie up $200K+ in revenue, and fragmented workflows from intake to billing create chaos.
CERTIFY Health’s unified platform, covering patient experience, practice management, revenue cycle, payments, interoperability, and FaceCheck ID, transforms this with connected, end-to-end automation tailored to your size (solo to PE-backed).
This 12-week roadmap (14 weeks for solos) delivers phased adoption:
- Pre-Adopt for buy-in
- Pilot for quick wins (25-35% no-show cuts)
- Scale for full rollout (>90% clean claims)
- Sustain for habitual use
Proven for derm-specific pains like Mohs coding and cosmetics upsells.
Ready to unlock $200K and streamlined care?
Why Dermatology Practices Need Unified Platforms Now
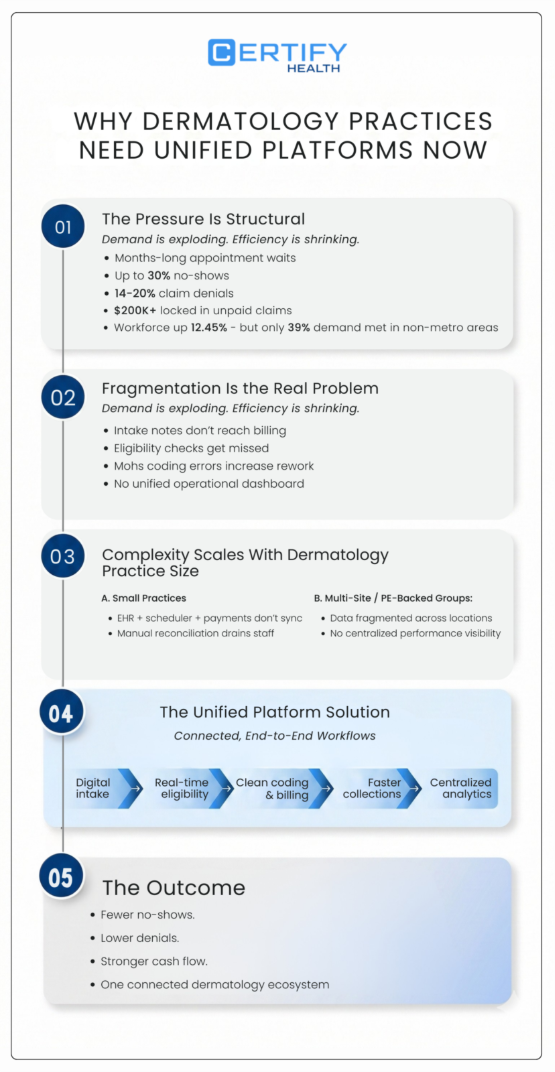
Dermatology hospitals today face exploding demand but crumbling efficiency. Patients wait months for appointments, while no-shows waste prime-time slots. Fragmented communication means intake notes never reach billing, leaving managers staring at revenue black holes.
The pressure is structural, not seasonal.
The dermatology workforce is growing (about 12.45%), yet in non-metro regions, only about 39% of patient demand is being met. Capacity gaps are widening while operational inefficiencies compound the strain.
The numbers make it urgent:
- No-show rates can reach 30%, draining schedules and revenue.
- Claim denials hover between 14–20%, often due to Mohs coding errors and missed eligibility checks, tying up cash and increasing rework.
- Unpaid claims can lock up $200,000+ in outstanding revenue.
And complexity scales with size.
In solo and small practices, disconnected EHRs, schedulers, and payment apps create workflow friction.
In multi-site dermatology groups and PE-backed hospitals, the challenge is data fragmentation across locations, with no unified operational view.
Unified platforms transform dermatology practice by creating connected, end-to-end workflows, from patient intake to eligibility checks, billing, and collections, keeping both patients engaged and revenue flowing.
This guide delivers a unified platform adoption framework built specifically for dermatology hospitals, helping transform fragmented communication into connected healthcare systems.
Journey Through Care: Where Fragmentation Hurts Most
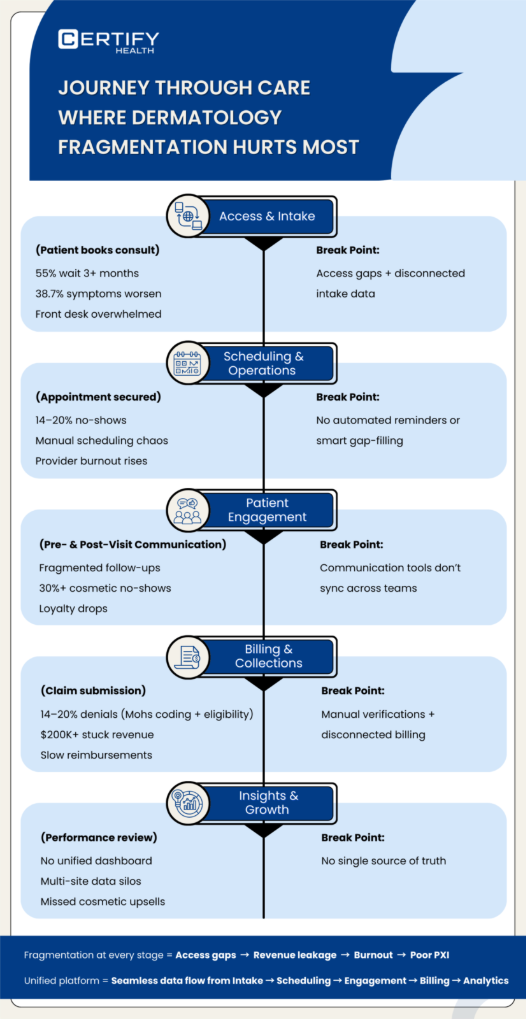
Walk with me through a typical patient care journey at your dermatology hospital. It starts smooth… then shatters.
Getting Patients In
New consults drag, 55% wait over 3 months (avg 2.5), with 38.7% worsening symptoms. Front desk fields endless calls chasing spots; managers watch access gaps bleed revenue as non-metro demand outstrips 12.45% supply growth.
Scheduling & Operations
Manual books amplify 14-20% no-shows (industry avg), with 24% of dermatologists calling “difficult patients” their top headache. Providers burn out on drama; managers scramble to fill eroded schedules.
Keeping Patients Engaged
Fragmented communications spike no-shows in cosmetics; spotty follow-ups tank loyalty. Extenders (PAs/NPs) fight workflow chaos; billers miss collections on ghosted repeats.
Billing and Collections
14-20% denials from Mohs coding, manual insurance verifications, cash flow crawls. Billers live in denial dread; C-suite frets over stuck capital.
Insights & Improvement
Siloed insights blind upsells (cosmetics) and PXI; no unified view across sites. Everyone pays the price for operational blind spots.
Intake data ghosts billing? Access gaps persist despite growth? That’s fragmentation in action. Unified platforms bridge with seamless data flow, but adoption needs a plan.
Unified Platform Framework for Dermatology Hospital Practice Transformation

Unified systems rarely fail due to capability gaps; they fail when user adoption never takes hold.
In dermatology hospitals, new systems often get introduced with urgency, but without alignment. Front desk teams feel overwhelmed. Billing teams fear disruption. Providers worry it will slow them down. When adoption is forced instead of earned, even the best unified platform struggles.
Our practice transformation guide is designed to prevent that.
It draws from proven behavioral science frameworks, including the Technology Acceptance Model (TAM), the Unified Theory of Acceptance and Use of Technology (UTAUT) framework, and agile change principles, but adapts them specifically for dermatology workflows.
At its core, adoption begins with two simple questions staff subconsciously ask:
- “Will this actually make my job easier?” (Perceived Usefulness)
- “Can I use it without frustration?” (Ease of Use)
For dermatology hospitals, usefulness means fewer no-shows, faster eligibility checks, cleaner Mohs coding, and predictable collections. Ease of use means intuitive scheduling, simplified intake, and front-desk-friendly workflows.
Beyond individual perception, broader organizational forces influence behavior. Performance expectancy (clear RCM ROI), effort expectancy (low learning curve), social influence (peer adoption across locations), and facilitating conditions (hands-on training and support) all shape long-term utilization.
But intention alone isn’t enough.
That’s where ARC principles come in — structured, agile cycles that focus on:
- Imagine: Define measurable operational wins
- Educate: Equip teams with practical, role-based training
- Validate: Prove early results (e.g., intake completion lift by Week 3)
Instead of a “big bang” rollout, the model progresses through four deliberate stages:
Pre-Adoption → Pilot → Scale → Sustain
Moderators such as practice size, ownership structure, and procedural mix (medical dermatology, Mohs, cosmetics) influence pacing. A solo practice may need hands-on reassurance. A PE-backed group may accelerate through social proof and performance metrics.
Success isn’t declared at go-live. It’s measured through utilization benchmarks, workflow compliance, and financial impact.
When adoption is structured, measurable, and aligned with real dermatology tasks, unified platforms don’t just launch; they stick.
CERTIFY Health: The Unified Platform Built for Dermatology Hospitals
CERTIFY Health is a unified platform built for dermatology hospitals like yours. It’s not another band-aid app; it’s a connected ecosystem that brings together patient experience, practice management, patient management, revenue cycle management, interoperability, and secure authentication into one seamless workflow.
From digital intake and self-scheduling to clinical coordination, eligibility checks, automated billing, and enterprise-level analytics, CERTIFY Health ensures every touchpoint, patient-facing and operational, works as one connected system. Whether you’re a solo dermatology practice or a multi-site organization like U.S. dermatology partners, the platform scales without fragmenting your data or workflows.
Key superpowers:
- Patient Experience (PXP): Digital intake, self-scheduling, automated reminders
→ 25–35% fewer no-shows. Higher NPS.
- Practice Management System (PMS): Smart scheduling, resource optimization, role-based dashboards
→ 15–20% operational efficiency lift.
- Patient Management: Centralized records, treatment tracking, coordinated follow-ups
→ Better care continuity. Stronger adherence.
- Revenue Cycle Management (RCM): Real-time eligibility, Mohs coding support, denial reduction
→ >90% first-pass claims. Predictable cash flow.
- CERTIFY Pay (Embedded Payments): Text-to-Pay, payment plans, automated collections
→ 40–60% faster collections. Higher point-of-service revenue.
- Interoperability + FaceCheck Security: EHR integrations, multi-site sync, secure authentication
→ Seamless data flow. Faster, safer check-ins.
CERTIFY Health turns fragmented communication into connected workflows, proven in solo medical practices to PE giants.
Detailed 12-Week Unified Healthcare Platform Implementation Guide
Deploy CERTIFY Health’s unified platform in phases to ensure smooth adoption. Track performance through clear benchmarks: NPS above 70, no-shows under 10%, and claim acceptance rates exceeding 90%, to confirm operational and financial improvement.
Stage 1: Get Everyone On Board (Weeks 1-2)
Goal: Fix resistance and spot your clinic’s weak spots in patient intake and payments.
- Map your team: Find supporters (like practice managers) and doubters (like doctors). Hold a kickoff meeting: Ask, “Are claim denials eating 14-20% of your profits?”
- Show quick ROI: Instantly calculate the financial impact of reducing no-shows and lowering claim denials. See how CERTIFY Health unlocks $200K+ in revenue by Booking a Demo.
- Demo it: Run a 5-minute simulation of CERTIFY Health’s patient intake. Walk through a real patient journey to reveal communication gaps.
- Audit readiness: Check your current tech (e.g. EHR systems). Outline how CERTIFY Health aligns with and integrates into each clinic location. Aim for 80% team buy-in.
- Next step: Get a signed greenlight document with your ROI numbers.
Trigger to move on: Team sees how fragmented patient communications hurt care.
Stage 2: Test and Prove It Works (Weeks 3-6)
Goal: Deliver fast wins in patient intake and scheduling.
- Start small (MVP): Turn on CERTIFY Health patient intake + scheduling engine. Scan forms with OCR, auto-fill patient info, let them self-book. Expect 25-35% fewer no-shows.
- Gather feedback: Send weekly surveys (aim for NPS score >70). Test A/B: Manual reminders vs. CERTIFY Health automated text reminders.
- Train easily: 1-hour sessions per role. Staff loves the simple interface—no steep learning curve.
- Wins to celebrate: Patients stay engaged with auto-texts. Front desk saves 15 hours/week.
Checkpoint: 85% satisfaction? Expand to patient engagement and billing.
Stage 3: Roll Out Everywhere (Weeks 7-12)
Goal: Make CERTIFY Health part of every workflow across sites.
- Automate payments: Add Text-to-Pay and insurance checks upfront. Speed collections by 40-60%.
- Go full steam: Activate RCM dashboards, sync all sites, train extenders on seamless workflows.
- Build momentum: Spotlight champions sharing wins like “No-shows dropped 30%!”
- Track success: Hit >90% first-pass claims. Ensure all data flow smoothly.
Pro tip: Weekly 10-minute standups link wins to role; billers cheer fewer denials.
Checkpoint: Key metrics green? You’re live.
Stage 4: Make It Stick and Improve (After Week 12)
Goal: Turn CERTIFY Health into a habit and keep optimizing.
- Monitor loyalty: Use CERTIFY Health analytics for >85% patient satisfaction.
- Quarterly check-ins: Ensure >80% feature use. Tweak based on staff feedback.
- Grow it: Add cosmetics upsell tools
- Handle risks: For solo docs, extra front-desk training. For multi-site, use pilot leaders for consistency.
Your Practice Transformation Starts Here. See Results. See ROI.
Sub-Specialty & Size-Specific Rollouts in Derm
CERTIFY Health flexes for your dermatology hospital profile. Timelines: 12 weeks base, adjusted slightly.
1. Solo/Small Dermatology Hospital (1-3 Doctors, Manual Paperwork Chaos, No IT Team)
Why it fits: You handle everything alone. CERTIFY Health automates patient intake, scheduling, documentation, billing, insurance checks, system connections, and payments without needing tech experts.
Total Timeline: 14 Weeks (extra time to build trust).
| Stage | Weeks | Implementation Roadmap: Key Actions & Ownership | Expected Wins & Trigger to Next Stage |
|---|---|---|---|
| Pre-Adoption | 1-3 | Practice Owner/Lead Doctor: Review no-show rates and claim denials. Demo patient experience platform (intake and FaceCheck identity verification). Calculate return on investment. | Spot $50,000 in lost revenue; owner approves in writing. |
| Pilot | 4-7 | Front Desk Staff: Turn on patient experience platform for scheduling, reminders, intake, form scanning, plus patient management for documents. Test on real patients. | Save 15 hours per week; errors drop 20%. Patient satisfaction scores over 70. Move to Scale. |
| Scale | 8-11 | Practice Owner/Lead Doctor + Biller: Add practice management system workflows, revenue cycle management for billing, CERTIFY Pay for text-to-pay, and interoperability setup to connect electronic health records. Train everyone. | Unlock $200,000 in revenue; 90% of claims are approved first time. |
| Sustain | 12-14 | Practice Owner/Lead Doctor: Check performance dashboards weekly and make small tweaks based on data. | All features become daily habit → Fully automated practice life. |
Pro Tip: Train just 1 front desk person first; the interface is simple, like using a phone app.
2. Mid-Size Groups (4-10 Doctors, Fighting Claim Denials Daily)
Why it fits: Denials eat profits. CERTIFY Health cuts them with accurate patient ID and checks.
Total Timeline: 12 Weeks (longer pilot to prove accuracy).
| Stage | Weeks | Implementation Roadmap: Key Actions & Ownership | Expected Wins & Trigger to Next Stage |
|---|---|---|---|
| Pre-Adoption | 1-2 | Practice Manager + Doctor Leads: Map revenue leaks per clinic site. Demo FaceCheck identity verification with proof-of-concept sites. | Cut patient calls by 30%; full team agrees to proceed. |
| Pilot | 3-6 | Front Desk Staff + Billers: Activate patient experience platform for scheduling, reminders, forms, FaceCheck identity checks, plus basic patient management documents. Run A/B tests. | Denials drop 13.5%; add 2 visits per week. 85% staff satisfaction. Move to Scale. |
| Scale | 7-10 | IT/Admin Staff: Connect practice management system and electronic health records (interoperability), full revenue cycle management, CERTIFY Pay. Train all roles. | Cash collected 40% faster; coordination smooth across team. |
| Sustain | 11-12 | Practice Manager: Review performance dashboards from patient experience to revenue cycle management. Spot cosmetics upsell chances. | Efficiency rises; Mohs surgery coding works better with clean data. |
Pro Tip: Test manual reminders vs. CERTIFY Health auto-reminders for each doctor.
3. Large/PE-Backed Dermatology Hospital (10+ Doctors, Multi-Site Like US Derm Partners)
Why it fits: Siloed data across sites hurts. CERTIFY Health unifies everything fast.
Total Timeline: 12 Weeks (parallel pilots on multiple sites).
| Stage | Weeks | Implementation Roadmap: Key Actions & Ownership | Expected Wins & Trigger to Next Stage |
|---|---|---|---|
| Pre-Adoption | 1 | Executives + Site Leaders: Map losses across all sites. Calculate return on investment for patient experience platform and FaceCheck. | Return on investment clear; buy-in by end of week 1. |
| Pilot | 2-5 | Pilot Site Teams: Launch patient experience platform intake, scheduling, check-in with FaceCheck, plus patient management on 20% of sites. | Cut no-shows 25-35% chain-wide. Key metrics green? Move to Scale. |
| Scale | 6-10 | IT Team + Trainers: Roll out full practice management system, revenue cycle management, dashboards, CERTIFY Pay to all sites. Set up interoperability with FHIR/HL7 standards to Epic or Cerner systems. | 90% claims approved first time; save 60-80% appointment cancels. |
| Sustain | 11-12 | Central Operations Team: Track chain-wide performance + quarterly audits. | Boost patient retention; acquisition data flows seamlessly. |
Pro Tip: Pilot on 3-5 sites at once, use their success stories for faster buy-in.
4. Cosmetic-Heavy Practices (Any Size, Botox/Fillers Revenue Focus)
Why it fits: No-shows kill elective income. CERTIFY Health fills slots and tracks repeat visits.
Total Timeline: 12 Weeks (start with engagement tools).
| Stage | Weeks | Implementation Roadmap: Key Actions & Ownership | Expected Wins & Trigger to Next Stage |
|---|---|---|---|
| Pre-Adoption | 1-2 | Practice Manager + Aesthetician Leads: Map where patients drop off. Demo patient experience platform engagement tools. | Agree no-shows are revenue poison. |
| Pilot | 3-5 | Front Desk Staff: Launch patient experience platform booking, check-in, FaceCheck, plus patient management for consent forms and documents. | Fill 100% of slots; patient satisfaction up 25%. Repeat visits rising? Move to Scale. |
| Scale | 6-9 | Billing Team: Add cash-pay revenue cycle management, CERTIFY Pay for recurring or auto-payments, practice management system tracking, interoperability for injectables data. | Payments 40% faster; repeat visits up 30%. |
| Sustain | 10-12 | Practice Manager: Check loyalty trend dashboards. | Lock in patient loyalty; turn data into cosmetics sales intel. |
Pro Tip: Pilot high-dollar services like Botox slots first.
Conclusion
This roadmap turns dermatology chaos into connected efficiency, fewer no-shows, cleaner claims, flowing revenue, and engaged patients across solo clinics to multi-site empires.
CERTIFY Health isn’t just software; it’s your 12-week path to practice transformation, with type-specific tweaks ensuring adoption sticks.
Book a CERTIFY Health demo now to map your gaps and unlock $200K in Weeks 1-2.





















