Table of Contents
Ophthalmology practices today face structural strain, rising no-show rates (38%), denial rates reaching 13%, A/R cycles stretching beyond 40 days, and fragmented imaging data creating compliance and workflow gaps. Staffing shortages and disconnected systems only intensify the pressure.
This Technology Adoption Guide outlines a structured, size-aligned rollout of a unified ophthalmology platform powered by CERTIFY Health. By integrating Patient Experience, Practice Management, Patient Management, Interoperability, Revenue Cycle Management, Payments, and enterprise-grade Security into one ecosystem, practices eliminate data silos and reduce administrative burden.
A phased 12-week implementation minimizes disruption while delivering measurable impact: no-shows reduced below 10%, denials under 5%, A/R cycles under 30 days, and 10–15% operational efficiency gains.
With role-based training, performance dashboards, and structured governance, adoption becomes controlled, not chaotic.
Book a Demo with CERTIFY Health to see how unified execution transforms your ophthalmology practice.
The Reality Facing Every Ophthalmology Practice

Today’s Ophthalmology practice is under structural pressure, operationally, financially, and technologically.
- No-show rates average 21.7%, rising to 38% for long-scheduled appointments.
- Exam chairs sit empty while demand grows. Patient waits stretch from 43 ± 38 minutes in waiting rooms.
- Meanwhile, Ophthalmology RCM struggles. Denial rates range from 13%, and 65% of denied claims are never resubmitted. A/R days linger between 25–45. Revenue leaks quietly.
- Behind the scenes, Data silos compound the problem. Nearly 75% of imaging data lives outside core systems, forcing duplicate entry, workflow gaps, and compliance risk.
- Stack on workforce pressure: ophthalmologist supply is projected to fall 12% by 2035 while demand rises sharply, widening care gaps, all while fragmented tools intensify training demands and operational overload.
These are not isolated inefficiencies. They are symptoms of fragmentation inside the modern Ophthalmology medical practice.
If these numbers look familiar, it’s time for structural change.
Schedule a CERTIFY Health Strategy Demo.
Why a Unified Approach Is No Longer Optional
Traditional point solutions add complexity. What practices need instead is Ophthalmology practice management software that connects workflows end to end.
The right Software for ophthalmology practice eliminates system hopping, reduces manual tasks by 10–15%, and restores visibility across the operation.
A modern Ophthalmology software platform must unify:
- Patient experience
- Practice management
- Patient management
- integrations
- Revenue cycle management
- Authentication and security
When these components operate inside one ecosystem, silos collapse, staff efficiency improves, and governance becomes manageable, especially under a centralized governance model for multi-site groups.
Ophthalmology Guide for Tech Adoption by Practice Size
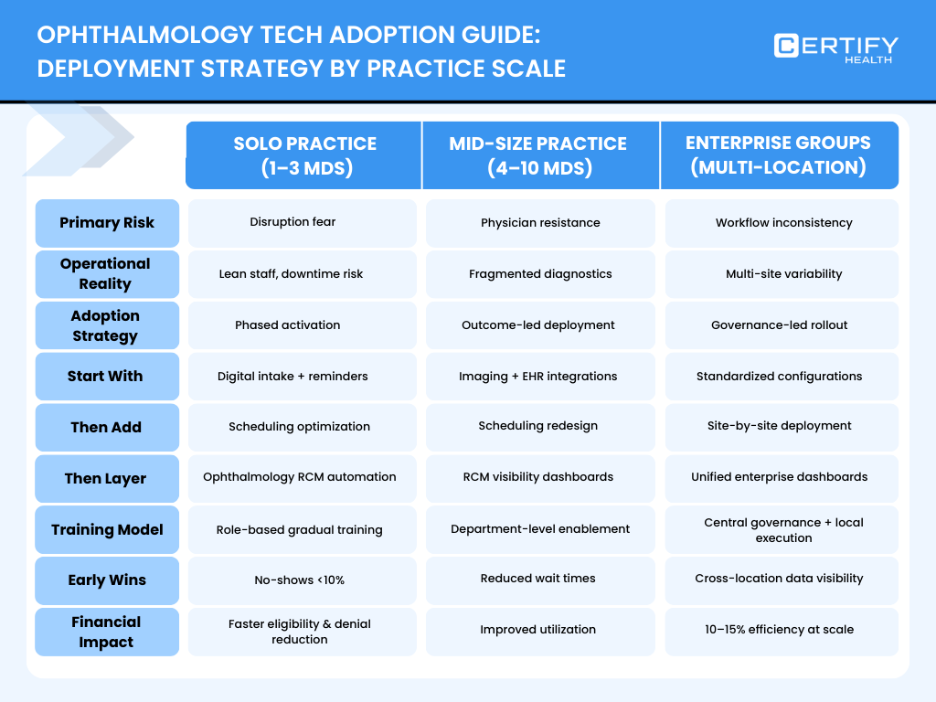
Technology adoption fails when rollout ignores operational reality. This Ophthalmology guide aligns deployment strategy with practice scale.
Solo Ophthalmology Practice (1–3 MDs)
A Solo ophthalmology practice operates with limited staff capacity and high downtime risk. Owners fear disruption more than inefficiency.
The solution: Phased rollout.
Instead of full system replacement:
Phase 1: Activate Patient experience tools (digital intake + reminders)
Phase 2: Layer scheduling optimization under Practice management
Phase 3: Introduce Ophthalmology RCM automation
This structured activation reduces training overload and builds quick KPI wins.
With Role-based training:
- Front desk focuses on intake and scheduling
- Billers train on Ophthalmology billing software workflows
- Providers adapt gradually to Patient management enhancements
Result:
- No-shows drop below 10%
- Check-in time falls under 10 minutes
- Denials decline quickly with automated eligibility
Confidence grows before complexity does.
Mid-Size Ophthalmology Practice (4–10 MDs)
Growing practices face physician resistance, fragmented diagnostics, and rollout fatigue.
Here, the focus shifts to measurable outcomes.
Demonstrate value early using performance dashboards:
- Reduced wait times
- Improved utilization
- Denial reduction
Begin with integrations, connecting imaging and EHR systems, then redesign scheduling workflows.
Role-based training separates:
- Clinical flow (MDs)
- Front-desk operations
- Revenue cycle management teams
This targeted enablement prevents operational paralysis while increasing adoption speed.
Enterprise Ophthalmology Medical Practice Groups
Large multi-location groups face a different threat: inconsistency.
Without a centralized governance model, each location creates its own workflows, compliance risk multiplies, and data silos deepen.
Adoption strategy here includes:
- Site-by-site deployment
- Shared configuration standards
- Unified Performance dashboards across locations
- Enterprise-level Authentication and security
Integrations consolidate EHR and imaging data across all sites, eliminating fragmentation.
The outcome is sustainable 10–15% operational efficiency gains at scale.
See how CERTIFY Health aligns implementation to your exact practice size.
Book a Size-Specific Demo.
The Aii Framework for Technology Adoption
This ophthalmology guide draws inspiration from the change principles promoted by the American Academy of Ophthalmology.
The Aii model: Adoption, Implementation, Integration, ensures transformation sticks.
Adoption: Secure stakeholder buy-in using metrics: no-shows, denials, A/R days.
Implementation: Deploy modules in structured sequence – Patient experience, Practice management, Patient management, integrations, Revenue cycle management, Authentication and security.
Integration: Embed workflows into daily habits using role-based training and performance dashboards.
Technology alone does not create change. Structured adoption does.
Unified Platform Execution: How the Modules Interconnect
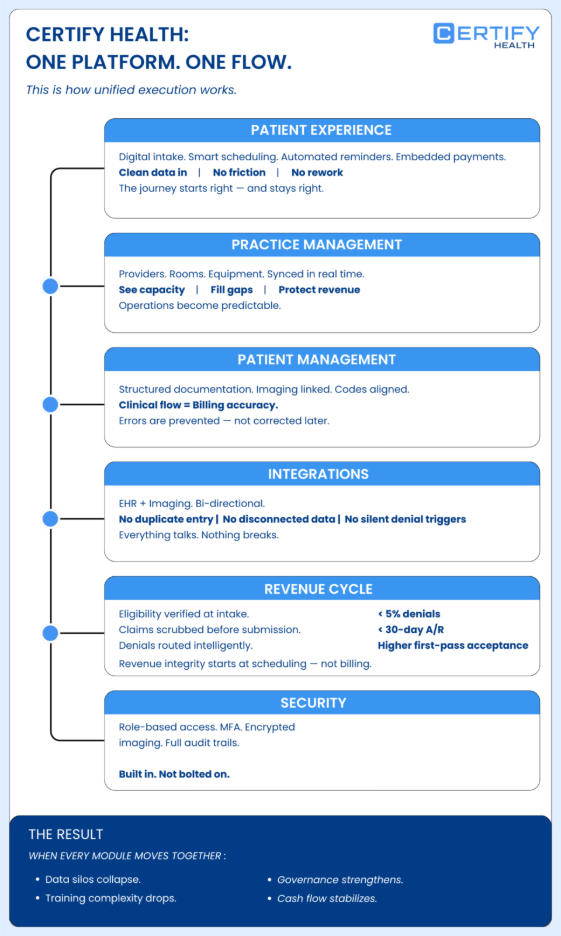
A true ophthalmology clinic software platform does not operate in layers, it operates as one system.
With CERTIFY Health, every module is designed to function as part of a unified architecture, not as disconnected tools stitched together over time.
Patient Experience
Digital intake, automated reminders, self-scheduling, and embedded payment tools reduce front-desk friction.
Data captured at the first touchpoint flows directly into Patient Management and Revenue Cycle Management — eliminating duplicate entry and reducing downstream errors.
With CERTIFY Health, the patient journey begins clean and stays clean through billing.
Practice Management
Smart calendars coordinate providers, diagnostic equipment, and exam rooms in real time.
Operational dashboards track occupancy, scheduling gaps, utilization, and performance metrics, giving administrators visibility into capacity and profitability.
This operational clarity feeds structured, accurate data into Ophthalmology RCM — improving claim precision before submission.
Patient Management
Structured documentation templates integrate exam findings, imaging references, procedure codes, and referral tracking.
Clinical workflows sync directly with billing logic, reducing coding discrepancies and preventing claim errors before they happen.
CERTIFY Health ensures documentation integrity supports reimbursement accuracy.
Integrations
Bi-directional integrations connect major EHRs and imaging systems, eliminating manual entry and improving coding accuracy.
Unified integrations reduce denial drivers before they occur.
Revenue Cycle Management
Modern Ophthalmology billing workflows within CERTIFY Health verify eligibility at intake, scrub claims before submission, categorize denials intelligently, and automate resubmission workflows.
A tightly connected Ophthalmology RCM engine can:
- Reduce denial rates below 5%
- Shorten A/R cycles to under 30 days
- Improve first-pass acceptance rates
- Strengthen cash flow predictability
Because revenue integrity starts at scheduling, not at billing.
Authentication and Security
Enterprise-grade authentication and security are embedded across the platform, including:
- Role-based access controls
- Multi-factor authentication
- Encrypted imaging protection
- Full audit trails
Security is not an add-on within CERTIFY Health. It is architected into every module.
Experience how the modules work together in real time.
Watch a Live CERTIFY Health Demo.
The Strategic Outcome
When Patient Experience, Practice Management, Patient Management, Integrations, Revenue Cycle Management, and Security operate inside unified ophthalmology practice management software powered by CERTIFY Health, fragmentation disappears.
- Data silos collapse.
- Training complexity decreases.
- Governance strengthens.
- Revenue stabilizes.
This is not just a better software. It is a structural reset for the modern Ophthalmology practice, executed through one unified platform
Implementation of Unified Healthcare Platform by CERTIFY Health | Aligned to Practice Size
| Phase | Weeks | Small (1–3 MDs) | Mid-Size (4–10 MDs) | Large (10+ MDs) |
|---|---|---|---|---|
| Foundation | 1–2 | • Pilot phase: launch digital intake and self check-in using multi-channel forms accessible via mobile, web, and in-office kiosks. • Staff onboarding (role-based training). • Baseline KPIs set (no-shows, A/R, eligibility match rates). |
• Infrastructure audit: subspecialty workflows (retina vs general ophthalmology), EHR/PM compatibility, multi-team kickoff. • Governance & workflows defined. |
• Enterprise IT readiness: VPN/sub-networks for shared configs, compliance audit, security baselines (HIPAA/SOC2/PCI). • Governance committee formation across sites. |
| Intake & Identity | 3–4 | • Activate multi-channel digital intake with instant insurance capture and eligibility checks. • Enable FaceCheck biometric ID capture at check-in (if used). |
• Add advanced patient intake workflows: biometric FaceCheck, consent e-signatures, photo ID capture. • Instant eligibility and benefits validation for every appointment. |
• Multi-location patient intake rules and identity governance. • Central administration of FaceCheck/consent policies with audit trails. |
| Scheduling & Engagement | 5–6 | • Deploy self-scheduling + ASAP List automation. • Activate automated reminders (SMS/email) to reduce no-shows. |
• Enhance multi-channel messaging, subspecialty templates, and provider-level feedback loop integration. • Expand scheduling rules for blocks, recurring slots. |
• Enterprise multi-location scheduling: cross-site waitlists, forecasting, and provider rotation optimization. |
| Payments & Billing (RCM) | 7–9 | • Launch CERTIFY Pay features: Text-to-Pay, automated co-pay capture, upfront balance presentation. • Enable denial dashboards with simple appeal workflows. |
• Introduce AutoPay enrollment, flexible payment plans, ERA auto-posting. • Set up automated claim-edit checks and monitor denial categories for accurate tracking and faster resolution. |
• Consolidated billing views and enterprise denial analytics. • Inter-site A/R transfers and centralized collections dashboards. |
| Patient Management & Clinical Workflows | 10–11 | • Deploy core charting tools and customized documentation templates designed specifically for ophthalmology workflows. • Set up basic performance dashboards (no-shows, collection rates). |
• Expand patient management: longitudinal timeline, SOAP/progress notes, care coordination tasks. • Add workflow automation for handoffs and task assignments. |
• Enterprise predictive analytics: no-show risk, productivity, payer trends; consolidated clinical dashboards. |
| Interoperability & Integrations | Ongoing | • Setup HL7/FHIR interoperability with existing EHR/PM systems. | • Deeper integrations: lab, imaging, and external referral loops. | • Governance of enterprise APIs, centralized connector libraries, analytics feed for enterprise reporting. |
| Go-Live & Continuous Optimization | 12 | • Full QA & KPI review (target: no-shows <10%). • Rapid support handoff. |
• End-to-end testing across subspecialties; staff refresher sessions. • Provider sign-off phasing. |
• Enterprise validation (audit trails, security cert). • Multi-site go-live & leadership review. |
CERTIFY Health customizes this phased rollout per ophthalmology practice size, minimizing training overload with training material and continued dedicated customer support.
Concerned about disruption? Let’s map your 12-week rollout plan.
Schedule Your Implementation Planning Demo.
ROI Metrics Breakdown
| Metric | Baseline (US Ophthalmology practice) | CERTIFY Impact | Annual Value ($2M Ophthalmology practice) | How CERTIFY Delivers |
|---|---|---|---|---|
| No-Shows | 20-38% | <10% via reminders/ASAP List™ | $200K+ revenue (e.g., 500 slots @ $400) | Patient experience automation recovers chair time. |
| Denials | 13% | <5% via scrubbing/eligibility | $150K+ clean claims (15% of $1M collections) | Ophthalmology RCM prevents 65% rework. |
| A/R Days | 40-60 | <30 via auto-posting | $400K working capital ($30K/mo cash flow) | Ophthalmology billing software accelerates cycles. |
| Efficiency | Manual entry (75% time) | 10-15% lift; 15-25 staff hrs/wk saved | $100K+ labor savings (20 hrs @ $50/hr) | Integrations + patient management cut duplicates. |
Software for ophthalmology practice like CERTIFY Health proves impact through measurable visibility. Performance dashboards track weekly KPIs, enabling leadership to adjust in real time rather than react months later.
Integrated workflows automate nearly 30% of administrative effort, while connected Ophthalmology RCM processes can elevate net collection rates toward 98% by reducing eligibility errors, coding gaps, and unworked denials.
Overcoming Barriers Step-by-Step
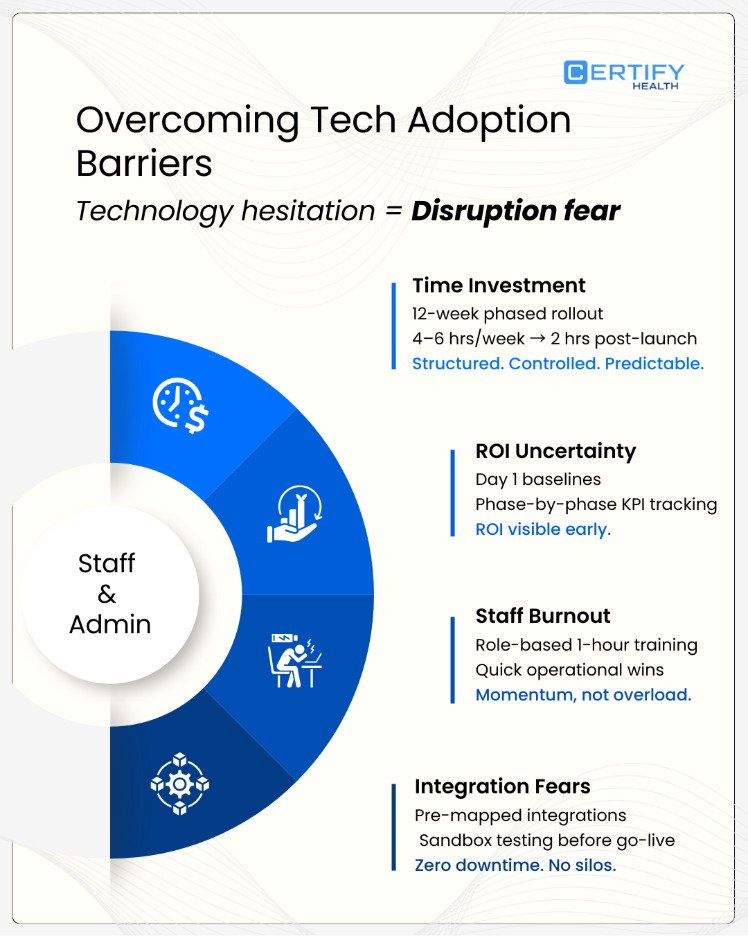
Technology adoption hesitation is rarely about software capability. It is about disruption risk. This Ophthalmology guide addresses that directly.
High Time Investment
A structured 12-week phased rollout reduces operational shock.
- Initial commitment: 4–6 hours per week during activation.
- Post-stabilization: approximately 2 hours weekly for optimization.
Defined milestones prevent chaos and maintain leadership visibility throughout the transition.
ROI Uncertainty
Baseline metrics are established on Day 1, for example, a current 25% no-show rate or 40-day A/R cycle.
Post-implementation KPIs are then measured phase by phase. Ophthalmology software supports this process with benchmark comparisons drawn from 500+ ophthalmology practices, giving decision-makers confidence grounded in data rather than projections.
Performance dashboards make ROI visible early, not retrospectively.
Staff Burnout
Training overload is a legitimate concern inside any Ophthalmology practice.
Instead of mass training events, role-based training breaks enablement into focused 1-hour modules tailored to:
- Front desk operations
- Clinical workflows
- Revenue cycle management teams
Quick wins, such as instant eligibility feedback during intake, create immediate friction reduction, reinforcing adoption momentum rather than fatigue.
Integration Fears
System disruption is often the largest psychological barrier.
Pre-mapped integrations connect to the majority of EHR and imaging platforms. Sandbox testing environments validate workflows before live activation, ensuring zero downtime during transition.
As integrations synchronize data flows across scheduling, documentation, and billing, data silos dissolve within a unified healthcare platform structure.
Conclusion
This Ophthalmology guide positions CERTIFY Health as essential ophthalmology clinic software for the modern Ophthalmology practice, not because it replaces tools, but because it connects them.
By aligning patient experience, practice management, patient management, integrations, revenue cycle management, and authentication and security inside one system, measurable gains occur without operational disruption.
- Phased rollout reduces risk.
- Performance dashboards prove ROI.
- Role-based training limits burnout.
Adoption becomes controlled, not chaotic.
The result: measurable operational improvement without unnecessary complexity.
Unify your workflows. Stabilize revenue. Scale with confidence.
Book Your CERTIFY Health Demo Now.





















