
Dental billing has distinct complexities that generic RCM tools are not designed for. CDT code coverage varies by plan. Annual maximums, frequency limitations, waiting periods, and coordination of benefits all affect what gets paid and how much the patient owes. When these variables are not verified before treatment, the result is denied claims, patient balance surprises, and revenue that takes months to collect.





CERTIFY Health dental patient communication software automates the messages that keep your schedule full and your patients engaged. Appointment reminders, hygiene recall campaigns, two-way text messaging, broadcast announcements, and post-visit review requests all run through one HIPAA-compliant platform connected to your dental EHR.
HIPAA Compliant
ASAP Waitlist Built In
24/7 Online Booking

A crown covered at 50% under one plan may be covered at 80% under another or not covered at all during a waiting period. Without real-time verification of CDT-specific coverage, treatment plans are presented with inaccurate cost estimates.
Patients who have exhausted their annual maximum are responsible for the full cost of remaining treatment. If staff do not check the remaining maximum before scheduling procedures, patients receive unexpected bills.
Dental practices that rely on paper statements or patient portal billing to collect balances see lower collection rates and longer days in A/R. Patients who do not pay within 90 days are unlikely to pay at all.
Multi-location dental groups need portfolio-wide visibility into denial rates, collection performance, and revenue trends by location. When each office manages billing independently, performance gaps go undetected.
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua.
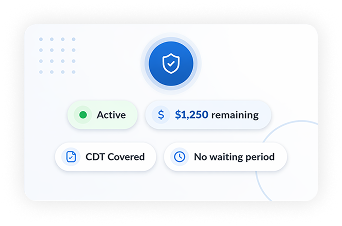
Real-time eligibility checks return active/inactive status, annual maximum remaining, frequency limitations, CDT code coverage, waiting period status, and coordination of benefits. Verification runs automatically for all scheduled patients.
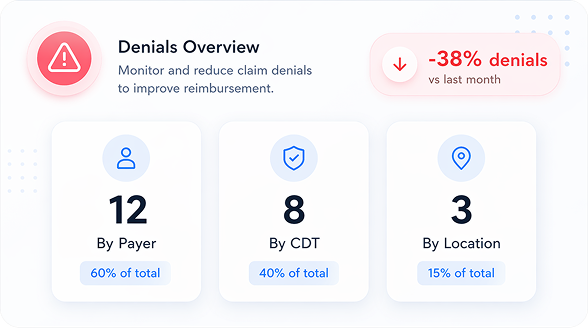
See how CERTIFY Health dental RCM software reduces denials, collects faster, and gives your billing team verified data before every procedure.

Yes. Insurance verification returns CDT-specific coverage details including coverage percentage, frequency limitations, and waiting period status for procedures.
Yes. Text-to-Pay sends patients a secure link to pay their balance from their phone. No portal login required.
Yes. CERTIFY Health integrates with Dentrix for patient data, insurance information, and payment posting. Verified eligibility data and payment receipts flow into the Dentrix patient record.
Centralized reporting gives DSO leadership visibility into financial performance across all locations. Standardized verification and collection workflows reduce variability between offices.
CERTIFY Health unifies Patient Experience, Practice Management, and Revenue Cycle Management – powered by FHIR/HL7 interoperability.





