Table of Contents
- Staff shortages are often workflow failures that waste time and revenue.
- Manual scheduling creates gaps that lead to lost income.
- Automation helps you see more patients without adding staff.
The Real Problem: A Vicious Revenue‑Cycle Cycle
Healthcare workforce shortages occur when the right people are not in the right place at the right time, limiting service capacity and operational performance.
Staffing shortages in hospitals and clinics create a slow boil for revenue.
Fewer people mean longer days, more overtime, and more dropped balls in billing and coding.
When front-desk staff are triple-booked, they miss timely claim submissions, extend eligibility checks, and delay patient follow-ups.
The result is healthcare revenue leakage. Appointments slip through cracks, denials pile up, and patient collections fall off.
What starts as a staffing challenge quickly becomes a revenue performance problem.
Simply put, every open FTE is a revenue-cycle risk, not just a staffing-office problem.
Healthcare Staff Shortage in Numbers
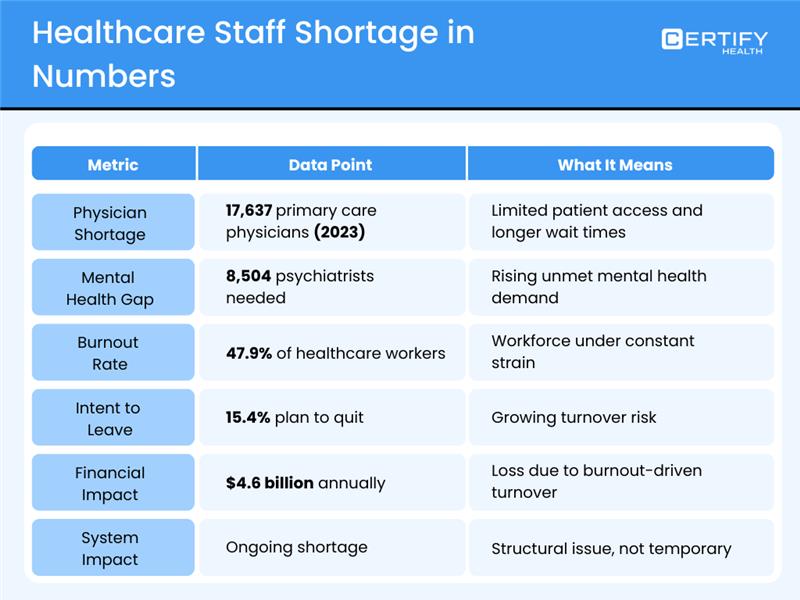
These numbers are not theoretical. They are already shaping your bottom line.
In 2023, the U.S. needed 17,637 primary care physicians and 8,504 psychiatrists to provide enough care in shortage areas.
When there are not enough providers, patient access slows, schedules tighten, and healthcare systems struggle to keep up with demand.
Without better workflows, this pressure will continue to grow.
Burnout is a major driver of the problem. A study found that 47.9% of workers felt burned out, and 15.4% planned to leave their jobs.
This leads to higher turnover and makes hiring even harder.
Burnout-related turnover is also expensive. It costs the healthcare system about $4.6 billion each year.
Together, these figures send a clear message: the healthcare staff shortage is structural, not temporary.
Manual Scheduling: The Hidden Revenue Killer

Manual scheduling is the quiet engine of this healthcare workflow crisis.
Paper calendars, Excel‑based rosters, and siloed phone trees create friction at every step.
Every time a front‑desk staff member double‑books a room, misreads a clinician’s block‑off, or misses a cancellation, the practice loses slot utilization and revenue.
Consider the ripple effect of a single missed slot over a year:
- A 15‑minute gap per day adds up to roughly 60 hours of unused provider time in a year.
- At typical visit rates, that can swing between $15,000–$30,000 in missed revenue per provider, depending on specialty.
This is not an error because of scheduling.
It is a systemic revenue‑leak tied directly to administrative burden in healthcare.
When staff are burned out, they are more likely to err on these tiny, repeatable tasks.
Burnout and Turnover: Why the Status Quo Fails

Burnout is not just a personal state. It is a workflow and operations problem.
Long hours, constant context‑switching, and manual data entry erode morale. For many clinicians, up to half of their day can be spent on paperwork instead of patient care.
This feeds the healthcare workflow crisis.
When staff are exhausted, they leave. Replacing them is costly and time‑consuming. Every onboarding cycle steals more peak‑revenue time from the practice.
The system compounds the problem.
More vacancies mean more overtime for remaining staff. More overtime deepens burnout. More burnout drives more turnover.
Until workflows are redesigned, any new hires simply refill a leaky bucket.
Why Hiring More Isn’t the Fix
Filling more open positions sounds like a straightforward answer to healthcare staff shortage.
In practice, it is not enough.
Many hospitals and clinics are already operating at or below capacity because they cannot staff safely.
More staff without better operations only increases labor costs.
If your scheduling is manual and your workflows are fragmented, you are paying more for the same inefficiency.
This is where healthcare operations management needs to shift from “people‑centric” to “process‑centric.”
The goal is not more bodies. It is fewer wasted motions per body. That is how you extract capacity from your current team.
Disconnected Tools and Calendar Chaos

Fragmented technology stacks make the healthcare staff shortage worse. Many clinics still juggle:
- Separate EHR, practice management, and scheduling tools
- Multiple calendars that do not talk to each other
When systems are disconnected, small errors happen every day.
A provider blocks time off in one system, but the front desk still sees that time as available.
A patient cancels an appointment, but the open slot is not visible to staff right away.
These gaps lead to scheduling conflicts, delays, and empty time on the calendar.
The result is missed opportunities, same-day cancellations, and poor use of staff and resources.
For schedulers, this is the true administrative burden in healthcare. Each switch between systems slows them down and drains productivity from an already stretched team.
Challenges revealed at HIMSS 2026 reinforced this reality.
Many organizations said disconnected systems still slow scheduling, delay patient care, and add work for staff.
Leaders said fixing these gaps is now a top priority to support staff and protect revenue.
The Solution: Digital Scheduling Systems
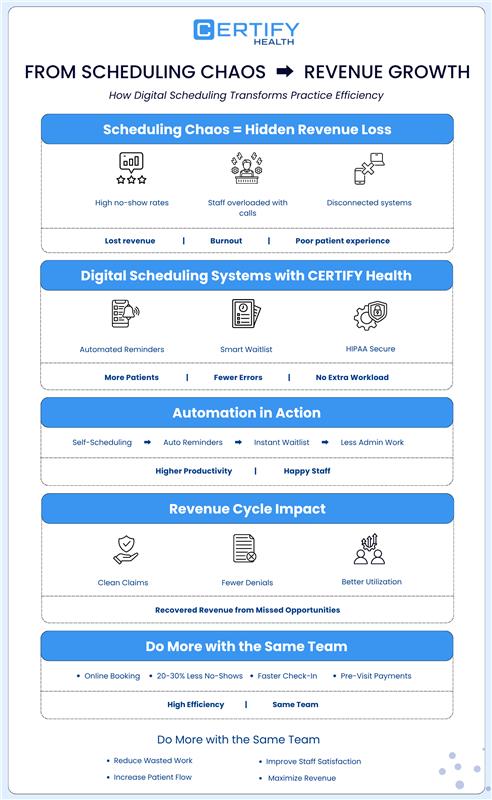
Digital scheduling systems cut through this chaos.
When you adopt automated patient scheduling software like CERTIFY Health, you are not just replacing a calendar. You are redesigning how your team works.
Key capabilities include:
- Real‑time calendar sync across EHR, rooms, and providers.
- Automated patient reminders (SMS, email, voice) to reduce no‑shows.
- Waitlist management tools that fill last‑minute gaps.
- HIPAA‑compliant scheduling software that integrates with existing workflows instead of creating new steps.
When these tools work together, staff can handle more patients without extra hours. This adds capacity without new hires.
How Automation Improves Medical Practice Efficiency
Automation directly targets the friction points in medical practice efficiency.
- Automated patient scheduling software reduces front‑desk calls by enabling self‑scheduling and online check‑in.
- Automated patient reminders improve attendance and reduce the need for manual follow‑up.
- Waitlist management fill cancellations faster, so slots do not sit empty.
From an operations view, automation takes over simple tasks, like calling patients to confirm appointments or rescheduling on paper.
This lets doctors and staff spend more time on important work, which helps patients and makes jobs more satisfying.
Connecting Scheduling to Revenue Cycle Optimization
Revenue cycle optimization cannot succeed in a scheduling black hole.
When appointments are missed, delayed, or miscoded, the RCM team inherits downstream chaos.
Modern scheduling tools plug directly into the revenue cycle.
- Real-time calendar sync helps ensure that booked visits match provider schedules and visit templates.
- Automated eligibility checks and pre-visit instructions save front-desk time and reduce last-minute denials.
- Data from scheduling also feeds analytics on appointment use, no-show patterns, and missed revenue opportunities.
This shifts healthcare cost strategies from cutting staff to getting more out of your existing team.
You are not reducing headcount, you are reducing wasted work and capturing revenue that might have slipped through the cracks.
Patient Engagement Tools That Scale Staff Capacity
Patient engagement tools are force multipliers for an understaffed team.
- Online booking portals let patients self‑schedule within defined rules, reducing call volume.
- Automated reminders cut no‑show rates by 20–30% or more in many specialties.
- Pre‑visit digital intake and payment prompts streamline front‑desk workflows and support collections.
These tools support—not replace—the human touch.
When staff are no longer drowning in repetitive tasks, they have more time for empathetic conversations and complex cases.
From a practice‑management perspective, this is how you run a high‑touch, low‑headcount model.
Implementation Roadmap: From Chaos to Clarity
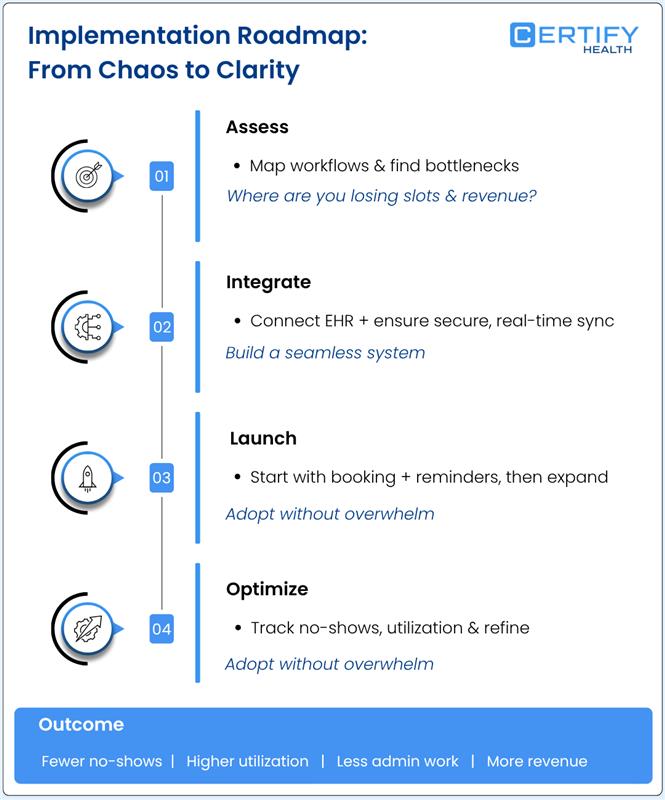
A successful rollout of a scheduling‑automation platform follows a clear, phased roadmap.
Assess current workflows
- Map all manual scheduling steps, calendars, and handoffs.
- Identify bottlenecks that correlate with missed slots and denials.
Define integration requirements
- Insist on real‑time calendar sync with EHR and practice‑management systems.
- Ensure HIPAA‑compliant scheduling software with secure data handling.
Phase in features
- Start with online booking and basic automated reminders.
- Add waitlist management tools and advanced templating once the team is comfortable.
Measure and refine
- Track no‑show rates, utilization, and front‑desk call volume before and after.
- Use analytics to tune reminder timing, visit templates, and slot rules.
Done right, this roadmap turns a technology project into a healthcare operations transformation.
Real‑World Wins: When Staffing Shortage Meets Smart Scheduling
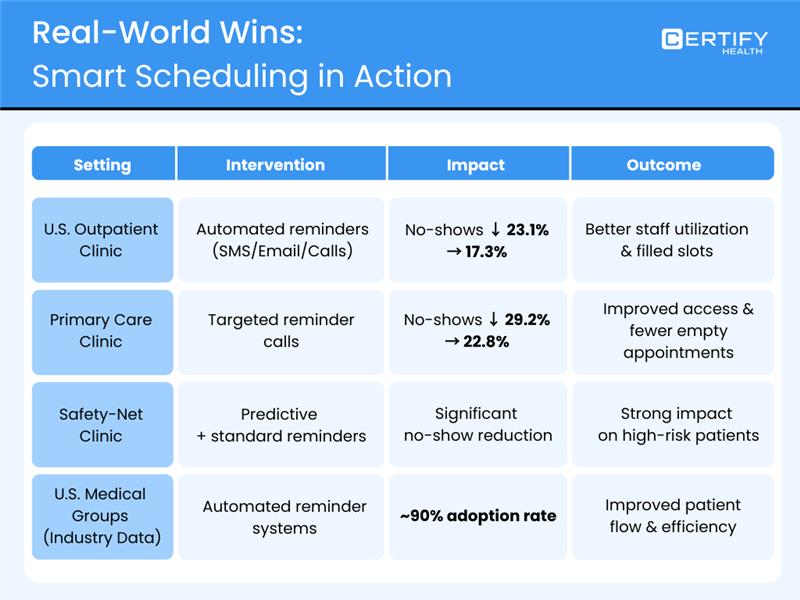

Clinics that invest in smarter scheduling see real results backed by U.S. research.
In one U.S. outpatient study, automated reminders cut no‑show rates from 23.1% to 17.3%, showing that scheduling technology helps more patients keep visits and makes better use of staff time.
At a major primary care clinic, targeted reminder calls reduced no‑shows from 29.2% down to 22.8%, freeing up appointments and improving access.
In a safety‑net clinic, adding predictive reminder calls to standard messaging led to significant reductions in no‑show rates, especially for high‑risk patients.
And industry data shows that nearly 9 in 10 U.S. medical groups today use automated appointment reminders because they help lower no‑shows and improve patient flow.
These results are not magic.
They happen when you stop trying to fix a healthcare staff shortage with more people and instead solve it with smarter workflow.
Conclusion
The healthcare staff shortage is real, structural, and revenue‑impacting.
But it does not have to be a death spiral.
Practices that modernize scheduling, automate reminders, and connect digital tools to revenue cycle optimization can unlock capacity from their existing teams.
If you are tired of running a healthcare practice on a skeleton crew, the next step is not another open job posting.
It is a deliberate redesign of how your staff works.
Ready to turn manual scheduling into a revenue‑enhancing workflow?
Let’s talk about how a HIPAA‑compliant scheduling platform and real‑time calendar sync can help your practice do more with less, while protecting staff well‑being and patient experience.






















