Table of Contents
It’s an exciting time to be at the intersection of healthcare and technology. As we move deeper into 2026, we’re seeing a profound shift in how information moves. We’ve spent decades digitizing records; now, the challenge is making that data speak to the right person at the right time.
Why Complete Healthcare Communications Is the New Infrastructure
We often talk about how information can be transformative when it’s organized and accessible. In healthcare, it is the fundamental infrastructure of care.
Fragmented communication is a clinical risk
For too long, we’ve accepted “silos” as a cost of doing business. But today, fragmented communication has become a primary clinical and financial risk.
When a specialist can’t see a primary care note, or a patient misses a follow-up because of a confusing text, the system breaks.
According to data, communication failures remain a leading root cause of sentinel events in US hospitals, highlighting the urgent need for a more integrated approach.

Defining Complete Healthcare Communications
When I think about “Complete Healthcare Communications,” I’m talking about a unified, intelligent layer that connects every touchpoint in the patient journey…from the first search for a doctor to the final bill payment.
We are living in an era of “distributed care.”
Patients no longer just visit a building; they engage via “digital front doors,” wearable monitors, and virtual clinics.
Their expectations have shifted; they expect healthcare to be as seamless as any other digital experience in their lives.
Today, I want to share a practical 6-step blueprint for health systems to move from fragmented noise to a synchronized, complete communication strategy.
What Is Complete Healthcare Communications?
To solve a problem, we first have to define it clearly. We need to move beyond “sending messages” to “orchestrating outcomes.”
A Simple Definition
Complete Healthcare Communications is the integrated exchange of clinical, operational, and financial data across all stakeholders to ensure safe, efficient, and personalized care delivery.
Core Pillars of Complete Healthcare Communications
- Patient Communication: Moving beyond reminders to proactive, two-way dialogue across the entire care continuum.
- Provider Communication: Ensuring the “handshake” between clinicians is instantaneous and data-rich.
- Operational Communication: Streamlining bed management, staff scheduling, and logistics to reduce “friction” in the system.
- Financial Communication: Providing transparent, easy-to-understand billing that respects the patient’s time and financial health.
- Compliance and Governance: Building on a foundation of privacy and security, thereby making sure every interaction stays within the guardrails of HIPAA and evolving federal standards.
What It Is NOT
It’s important to be clear about what this isn’t:
- It’s not just patient reminders: A text about an appointment is a start, but it’s not a strategy.
- It’s not just omnichannel messaging: Being everywhere is useless if the message is inconsistent.
- It’s not a marketing tool: While engagement is key, the primary goal is health outcomes and operational integrity, not just “brand awareness.”
The goal is to build a system that is helpful, helpful for everyone.
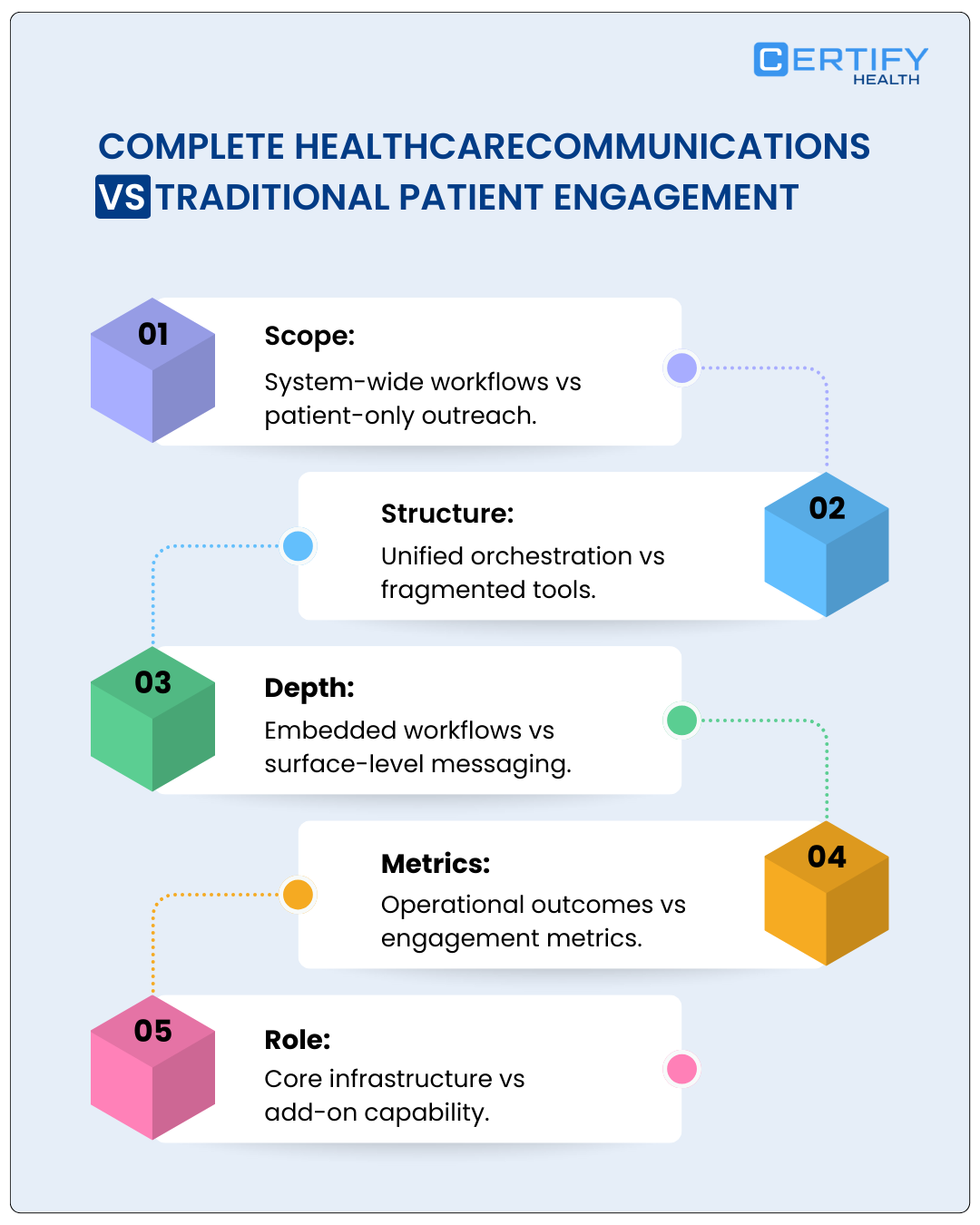
Why Fragmented Communication Is Costing Health Systems Millions
We are seeing a clear trend: fragmented systems create “dark data” and missed connections.
This is a systemic leak that impacts every line of the balance sheet.
Clinical Impact
When communication is siloed, the clinical consequences are immediate.
- Care Gaps: If a patient’s lab results don’t trigger an automated, easy-to-understand follow-up, that patient falls out of the system.
- No-shows and Readmissions: A patient who doesn’t understand their discharge instructions (or can’t easily ask a clarifying question) is significantly more likely to return to the ER.
- Poor Care Coordination: According to the Centers for Medicare & Medicaid Services (CMS), ineffective care transitions are a primary driver of avoidable readmissions.
The lack of a “single source of truth” during a handoff is a vulnerability we can no longer afford.
Financial Impact
The “hidden” costs of silence are often the most expensive.
- Revenue Leakage: When patients find the scheduling or pre-auth process too difficult, they simply go elsewhere.
- Denials and Delayed Payments: Fragmented financial communication leads to “sticker shock” and billing disputes. If the patient doesn’t understand the cost early, the likelihood of collection drops.
- Staff Inefficiency: We see clinicians and admin staff spending hours on “phone tag” or manual data entry. That is time taken away from high-value patient care.
Patient Experience Impact
Today, the “consumerization” of healthcare is complete.
- Confusion Across Touchpoints: Receiving a text from one department, an email from another, and a paper bill from a third creates a sense of chaos.
- Lack of Trust and Loyalty: Trust is built on consistency. If a health system can’t remember a patient’s communication preferences, the patient begins to wonder if they can be trusted with their clinical history.
The Data Behind the Friction
To understand the scale, we must look at the authoritative benchmarks. The administrative burden isn’t just a feeling; it’s a measurable crisis.
| Administrative Burden: Research from the U.S. Government Accountability Office (GAO) and related federal analyses have consistently highlighted that administrative costs, including complex billing and insurance-related tasks, account for a significant portion of U.S. healthcare spending. This is often estimated to be near 25% to 30% of total hospital outlays. |
| The Cost of "No-Shows": On a national scale, the impact is multi-billion. Federal health data indicates that missed appointments don't just stall revenue; they disrupt the entire resource allocation of a facility, increasing the "per-patient" cost of delivery for everyone else. |
| Readmission Costs: Under the Hospital Readmissions Reduction Program (HRRP), the federal government continues to penalize hospitals for high rates of 30-day readmissions. For many systems, these penalties represent millions of dollars in withheld reimbursements. This is money that could be reinvested into innovation. |
The goal for the next decade is clear: we must turn communication from a liability into a core competency.
Building this new infrastructure requires a shift from thinking about “tools” to thinking about “systems.” It’s about creating a cohesive fabric that supports every interaction.
Here is how we move from the fragmented present to a complete future.
The 6 Steps to Building Complete Healthcare Communications
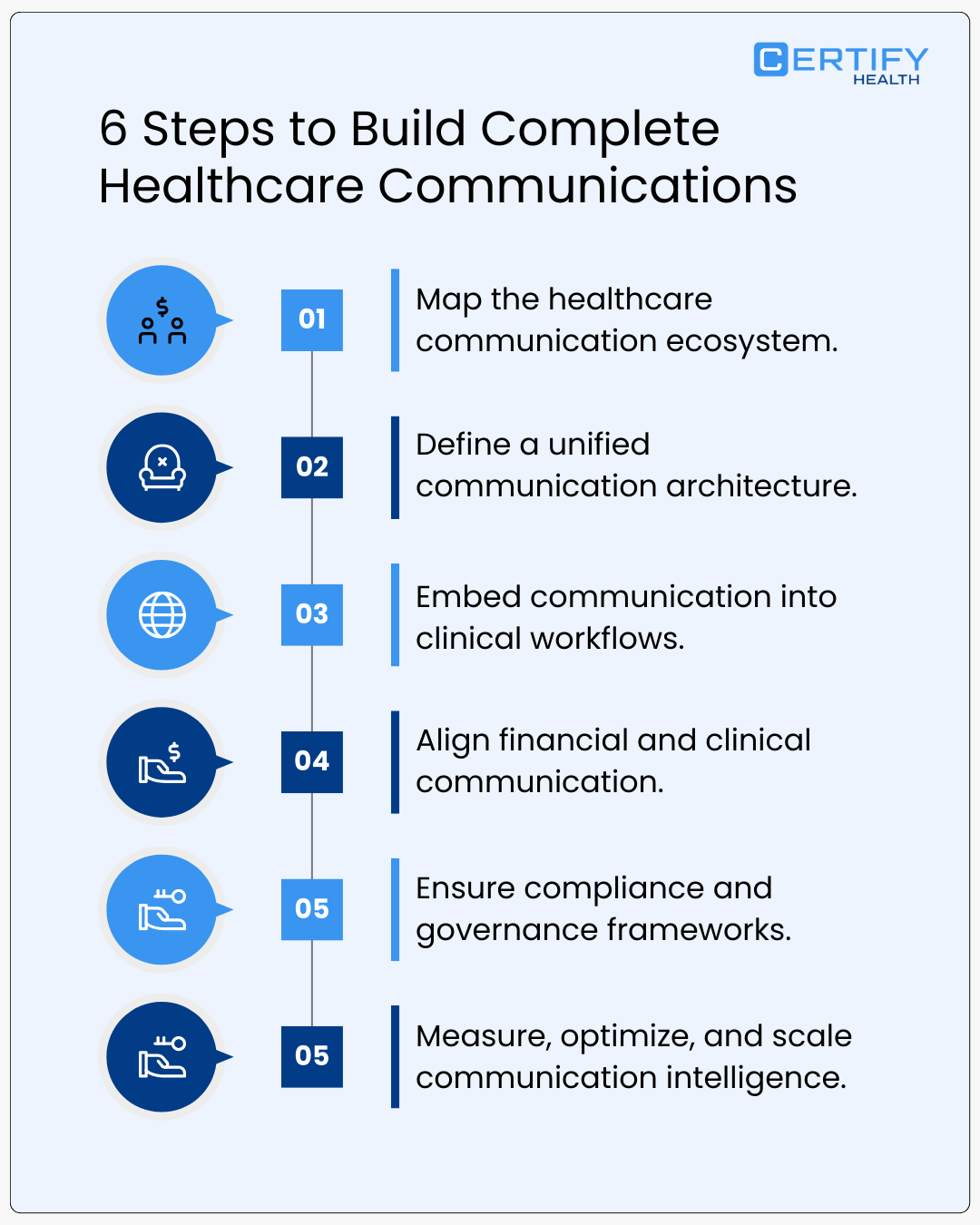
1. Map the Entire Healthcare Communication Ecosystem
You cannot optimize what you haven’t mapped. We have to look at the “user journey” in its entirety.
- Identify All Communication Moments: We look at the lifecycle from Discovery → Intake → Visit → Follow-up → Billing → Retention. Every one of these is a chance to provide value or lose trust.
- Include Every Stakeholder: It’s not just the patient. We must account for Providers, Admin teams, Payers, and Partners. If the admin team is frustrated, the patient will feel it.
- Audit Existing Tools and Silos: Most systems have a patchwork of EHR messaging, Call centers, SMS tools, and Billing systems. We need to see where the data gets “stuck.”
2. Define a Unified Communication Architecture
I often emphasize the “platform” approach. Healthcare needs a centralized layer to manage the noise.
Automating the transition from manual to unified digital clinical-administrative exchanges could save the U.S. healthcare system $18.3 billion annually by eliminating fragmented, non-orchestrated communication workflows
- Build a Centralized Communication Layer: Move toward a single orchestration engine where workflow-triggered communication ensures the right message goes out automatically when a clinical event occurs.
- Standardize Channels Without Losing Flexibility: Whether it’s SMS, Voice, Email, Patient portals, or Apps, the experience must feel like one conversation, not five.
- Align Clinical + Operational Messaging: Ensure that a clinical follow-up doesn’t conflict with an operational billing reminder. It should be one communication fabric.
3. Integrate Communications Into Clinical Workflows
The goal is to make the “right thing” the “easy thing” for clinicians.
- Embed Messaging into Care Pathways: Automate pre-visit prep and care plan adherence. If a patient needs to fast before a lab, the system should handle that reminder without a nurse picking up a phone.
- Reduce Staff Burden Through Automation: Use smart triggers and Automated workflows to handle routine queries. This allows humans to focus on the complex, empathetic work only they can do.
- Close the Loop With Feedback Mechanisms: True communication is two-way. Patient responses must feed directly back into the workflow so the care team can act in real-time.
4. Unify Financial and Clinical Communication
Financial stress is a clinical headwind. We must bridge the gap between “care” and “cost.”
- Connect Scheduling, Eligibility, and Payments: Provide pre-visit estimates and coverage clarity.
Technology should solve for cost transparency before the patient walks through the door.
- Reduce Billing Confusion: Use clear patient statements and real-time payment links.
If a patient can pay for a ride-share in one tap, they should be able to manage their healthcare balance just as easily.
- Improve Revenue Cycle Communication: Proactive denial alerts and self-pay workflows keep the system’s “oxygen” (revenue) flowing without manual chasing.
5. Ensure Compliance, Security, and Governance
In healthcare, privacy is of great significance.
- Build Communication Governance Frameworks: Use role-based access and audit trails to ensure data is seen only by those who need it.
- Align With Healthcare Regulations: Every interaction must be HIPAA-safe.
According to the Office for Civil Rights (OCR) at HHS, healthcare data breaches often stem from unauthorized access or insecure communication; governance is your best defense.
- Avoid Consumer Tool Pitfalls: Retail messaging tools aren’t built for the “high-stakes” nature of health data.
We need specialized, encrypted layers that respect the sanctity of the patient-provider relationship.
6. Measure, Optimize, and Scale Communication Intelligence
Finally, we move from being reactive to being predictive.
- Define KPIs That Matter: Track no-show reduction, response rates, and revenue acceleration. These are the true signals of a healthy system
- Use Communication Analytics: Identify journey bottlenecks through cohort analysis.
If one clinic has a 20% higher drop-off rate at the “Intake” stage, that’s a signal to investigate
- Move Toward Predictive Communication: Use AI-driven engagement timing to reach patients when they are most likely to respond.
By shifting to risk-based outreach, we can prioritize the most vulnerable patients before a crisis occurs.
This is how we build a more helpful healthcare system for everyone. It’s a journey from “sending messages” to “building connections.”
To realize this vision, we have to look closely at the “engine” under the hood. I’ve learned that the most powerful systems are the ones that are the most interconnected.
Technology Stack Needed for Complete Healthcare Communications
Building for the future requires a shift from “buying apps” to “architecting a platform.”
Must-Have Capabilities
- Workflow Orchestration: This is the “brain.” It ensures that a lab result doesn’t just sit in a portal but triggers an immediate, helpful notification to the patient.
- Deep EHR Integrations: Communication shouldn’t be a side-car; it must be natively aware of the clinical record. If it’s not synced with the EHR, it’s just noise.
- Omnichannel Delivery: Meeting users where they are—whether that’s a secure link, an encrypted app, or a simple voice call—while maintaining a single thread of truth.
- Automation + AI: We need systems that can handle the “80%” of routine interactions (rescheduling, prep instructions) so humans can focus on the “20%” that require deep empathy.
Build vs Buy Considerations
- Platform vs. Point Solutions: The era of the “single-feature app” is over. Adding ten different tools for ten different problems creates “integration debt.”
- Integration Cost Reality: The real cost of a tool isn’t the license fee; it’s the cost of making it talk to your other systems. A unified platform reduces this friction.
Role of Healthcare-Specific Platforms
Generic tools—the ones we use for retail or travel—simply aren’t built for the “high-stakes” nature of health.
They lack the HIPAA-grade security, the nuanced consent management, and the clinical context required to keep patients safe.
Common Mistakes Health Systems Make
Even with the best intentions, we see organizations fall into predictable “potholes.”
- Over-investing in channels, under-investing in orchestration: Having an app, SMS, and email doesn’t matter if they aren’t coordinated. It just creates “digital fatigue.”
- Ignoring financial communication: If a patient receives world-class clinical care but a confusing, “broken” bill three months later, the overall experience is a failure.
- Treating communication as marketing: While growth matters, the primary goal of this infrastructure is outcomes. If it feels like a sales pitch, patients will opt out.
- Lack of ownership across departments: Communication is often “homeless”—split between IT, Marketing, and Clinical. It needs a single owner who sees the whole journey.
- No measurable KPIs: If you aren’t measuring response rates or time-to-care, you’re flying blind.
The Future of Complete Healthcare Communications
As we look toward the end of the decade, the “helpful” system becomes the “proactive” system.
As of 2024, 65% of individuals in the U.S. were offered and actively accessed their online medical records or patient portals. This metric has more than doubled in the last decade (from 25% in 2014) and serves as the foundation for the next phase of ‘information fluidity.
AI-Native Communication Systems
We are moving toward Conversational AI that doesn’t just answer questions but anticipates them.
Imagine Autonomous follow-ups where the system checks in on a patient’s post-op pain levels and, based on the response, alerts a nurse or schedules a telehealth visit automatically.
Hyper-Personalized Patient Journeys
Communication will become context-aware. If the system knows a patient is a shift worker, it won’t call them at 10:00 AM.
It uses behavioral segmentation to deliver the right nudge at the exact moment it’s most likely to be effective.
Communication as a Clinical Asset
Ultimately, we will stop seeing communication as “admin” and start seeing it as a clinical asset.
Just like a diagnostic tool or a medication, the right information is a form of treatment.
According to the National Coordinator for Health IT (ONC), the goal of the next phase of interoperability is “information fluidity.”
When communication is complete, the system finally starts working for the people it was built to serve.
When we look at the complexity of these six steps, it’s clear that health systems shouldn’t have to build this from scratch. At Google, we believe in the power of platforms to solve systemic problems.
In the healthcare space, this is exactly where a solution like CERTIFY Health fits into the architecture of the future.
How Platforms Like CERTIFY Health Enable Complete Healthcare Communications
CERTIFY Health isn’t just another messaging tool; it’s a foundational layer designed to harmonize the “noise” into a single, coherent conversation.
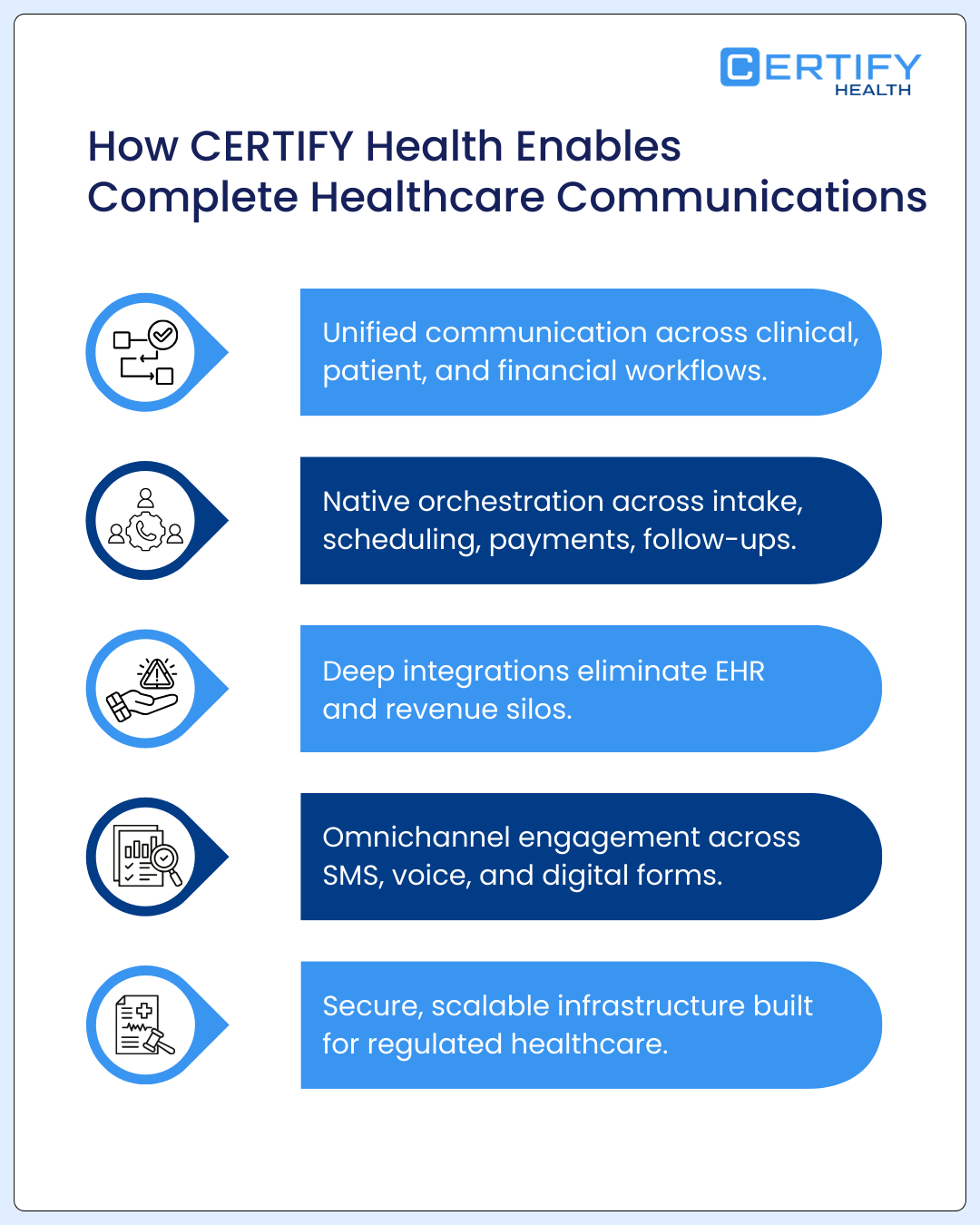
- Unified Communication Layer: It covers the entire care journey, ensuring that the transition from a digital check-in to a post-visit follow-up is seamless.
- Workflow-Native Communication: Unlike “bolted-on” apps, CERTIFY Health is built into the clinician’s existing workflow. This minimizes “toggle tax”—the cognitive burden of switching between different software screens.
- Deep EHR and System Integrations: It speaks the language of your core systems. By integrating deeply with the EHR, the communication becomes “context-aware,” knowing exactly where the patient is in their clinical pathway.
- Omnichannel Patient Engagement: Whether a patient prefers a secure portal, a text message, or an automated voice prompt, the platform ensures the experience is consistent across all touchpoints.
- Financial + Clinical Alignment: This is a critical differentiator. CERTIFY Health bridges the gap by linking scheduling and clinical prep with cost transparency and payments, reducing the friction that often leads to abandoned care.
- Automation with Intelligence: By utilizing smart triggers, the platform handles routine tasks like eligibility verification or appointment reminders, thereby freeing up staff for higher-touch patient needs.
- Built for Regulated Environments: Security isn’t an afterthought. The platform is designed specifically for the rigorous privacy and compliance standards required by federal oversight.
- Operational Visibility and Analytics: You can’t manage what you can’t see. CERTIFY Health provides the “dashboard” view of patient engagement, allowing leadership to identify and fix bottlenecks in real-time.
- Scalable Across Multi-Location Systems: Whether you are a single clinic or a massive multi-state IDN, the infrastructure scales without losing the personal touch that patients expect.
- Foundation for AI-Driven Healthcare: Most importantly, it creates the clean, structured data layer needed to implement the next generation of AI-driven, predictive outreach.
| Feature | Fragmented Communication (Traditional) | Complete Communication (CERTIFY Health) |
|---|---|---|
| Patient Onboarding | Manual forms; redundant data entry; phone-tag for insurance. | Digital intake & eConsent; automated biometric & eligibility verification. |
| Workflow Integration | Communication sits "outside" the EHR; manual clinical triggers. | Workflow-native; messaging is triggered by real-time EHR events. |
| Patient Engagement | One-way reminders; siloed portal messages. | Omnichannel 2-way messaging; automated feedback loops & education. |
| Revenue Cycle | Paper bills sent weeks later; high "sticker shock" & denials. | Real-time estimates & text-to-pay; unified clinical/financial alerts. |
| Staff Productivity | High "toggle tax"; multiple logins; heavy call volume. | Single orchestration layer; automated routine tasks (e.g., "ASAP" waitlists). |
| Security & Compliance | Risk of "retail" tool use; fragmented audit trails. | HITRUST/HIPAA certified; role-based access & centralized audit logs. |
| Clinical Safety | 80% of serious errors linked to handoff/communication lapses. | Standardized care pathways; closed-loop results & follow-up delivery. |
Conclusion
As we look at the landscape in 2026, the goal is simple but profound: we want to make healthcare as helpful as it is advanced. Communication is no longer a “soft skill” or an administrative byproduct; it is the infrastructure of trust.
By moving toward a Complete Healthcare Communications model, systems can reduce the administrative burden that, according to the U.S. Bureau of Labor Statistics (BLS), continues to drive high rates of burnout among healthcare support occupations.
When we fix the flow of information, we don’t just improve the bottom line—we improve the lives of the people providing and receiving care.
The technology exists to make healthcare feel human again. It’s time we put it to work.






















