Table of Contents
Introduction
75% of physicians report more prior auth denials over the past five years.
The fix? Using interoperability standards in healthcare and prior authorization automation.
That’s where FHIR comes in.
FHIR (Fast Healthcare Interoperability Resources) is a next-generation standard for healthcare data exchange. It helps systems share data through FHIR APIs. These APIs make FHIR data exchange fast and reliable.
Many leaders know what FHIR is. Its potential is widely recognized.
But most teams struggle with one thing: putting FHIR implementation to work in real workflows.
This blog bridges that gap.
Where FHIR APIs Fit in Your Prior Authorization Workflow
FHIR APIs connect systems for prior auth. They replace slow manual steps with fast FHIR data exchange.
Old workflows rely on faxes, phone calls, and web portals. These cause delays. They add extra work for staff.
FHIR data exchange sends data in real time. Teams move requests faster. They fix errors sooner.
Most organizations use hybrid workflows today. Providers may use FHIR in their EHR. Many payers still use X12 systems. Intermediaries bridge these systems through legacy system integration.
Here is how FHIR APIs support each step in the workflow.
1. Coverage Requirement Discovery (CRD): Check Requirements Early
A clinician orders a test. The system checks if prior auth is needed. This check runs inside the EHR using the CRD API.
Result: Staff know the rules early. They avoid extra requests.
2. Documentation Templates and Rules (DTR): Gather the Right Information
If auth is needed, the system pulls payer rules. It uses the DTR API. Required forms fill in with patient data automatically.
Result: Requests are complete. Delays drop.
3. Prior Authorization Support (PAS): Submit Requests Electronically
The PAS API sends clinical data directly to the payer. This replaces faxing and manual entry.
Result: Requests move faster. Teams track status in real time.
These faster workflows also help meet regulatory deadlines.
Under the CMS-0057-F rule:
- Urgent requests must be answered within 72 hours
- Standard requests must be answered within 7 days
Full FHIR vs. Hybrid Workflows
Full FHIR workflows connect directly to payer APIs. They can speed up approvals. But payer readiness still varies.
Because of this, many organizations use hybrid workflows during the switch. These models combine FHIR and X12. They support existing systems through healthcare API integration.
The right choice depends on your payer network, system readiness, and goals.
Did You Know?
Even with faster workflows, errors still drive denials.
According to an AMA study:
- 61% of physicians worry AI increases denials
- 93% report prior authorization delays
- 82% see patients abandon treatment due to auth issues
Speed alone is not enough. Requests must be complete, validated, and traceable.
CERTIFY Health addresses FHIR prior authorization challenges — rework, errors, and manual firefighting — with built-in checks and automation.
How the CRD → DTR → PAS Workflow Works (Step-by-Step)
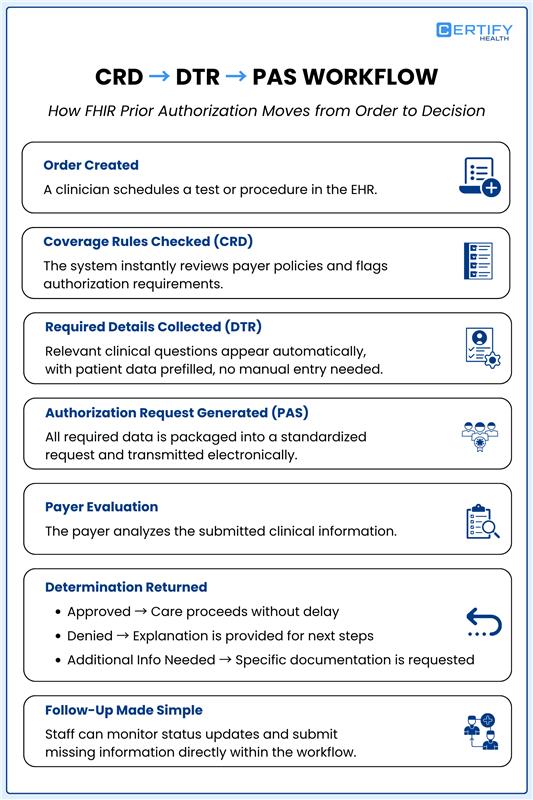
FHIR prior authorization becomes clearer when you walk through CRD, DTR, PAS together.
- The doctor orders a scan in the EHR
- CRD checks the rules — it finds a prior auth requirement
- DTR shows the form — patient data fills in automatically
- PAS builds the request and sends it to the payer API — structured and clean
The payer reviews the request and sends one of three responses:
- Approval — The order moves forward right away
- Denial — The payer explains the reason; the team can appeal
- Pending — The payer needs more information
If more documents are needed, DTR shows exactly what to submit next. Teams track updates in the system and respond quickly.
Pro Tip:
CERTIFY Health connects provider systems to payer prior authorization APIs using FHIR-based workflows. Staff can send requests, receive updates, and keep care on schedule.
FHIR Implementation: Key Decisions You Must Make
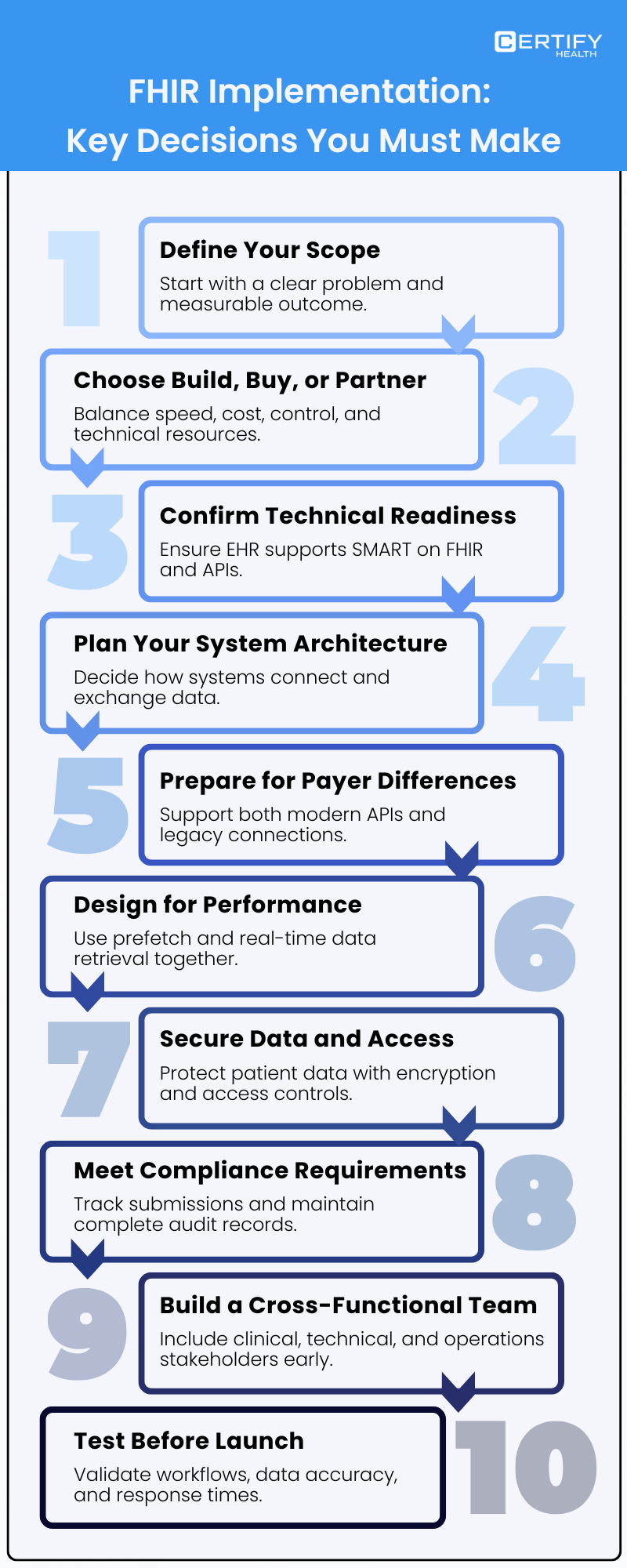
Every choice shapes your outcome. Here’s a simple way to evaluate each aspect.
Start With Scope
Define the problem first:
- Are you fixing delays?
- Reducing denials?
- Improving payer response times?
Clear goals guide every decision.
Build, Buy, or Partner?
- Build — Custom FHIR setup. Full control. But it takes time and skilled developers.
- Buy — Vendor tool. Faster start. Includes built-in workflows and FHIR compliance support.
- Partner — Use a health information network or integration platform. They manage payer API differences and connect your systems through healthcare API integration.
Check Your Technical Readiness
- Is your EHR ready for SMART on FHIR?
- Which FHIR version will you use? Most choose FHIR R4 — it is stable and widely supported.
- Does your data map cleanly? Legacy formats like HL7 and C-CDA must translate into FHIR resources. Inaccurate mapping leads to data gaps and delays in approvals.
Plan Your Infrastructure
Some organizations build a direct API layer. Others use middleware for healthcare API integration. Cloud platforms scale faster. Managed services reduce maintenance.
Prepare for Payer Variation
Not all payers support modern APIs yet. Build fallback paths for non-FHIR connections. Hybrid workflows keep requests moving and address healthcare interoperability challenges.
Focus on Performance
- Prefetch — Loads information ahead of time
- Real-time pulls — Delivers the latest data on demand
Many organizations use both.
Address Security and Governance Early
- Use secure login standards like SMART on FHIR
- Encrypt data during transfer
- Define clear rules for access and patient consent
- Use standard data formats to support FHIR data exchange
Stay Compliant and Audit-Ready
Track every submission. Log request times. Save response records. These steps support healthcare compliance and meet reporting needs under CMS-0057-F.
Build the Right Team
- Developers manage FHIR APIs
- Analysts validate workflows
- Clinical staff confirm documentation accuracy
Training helps teams adopt new steps faster.
Test Before Going Live
- Confirm data flows correctly
- Monitor response times and errors
- Fix issues early
Example: A provider group chose a vendor platform instead of building from scratch. They tested CRD connections first. Then they expanded to full workflow automation.
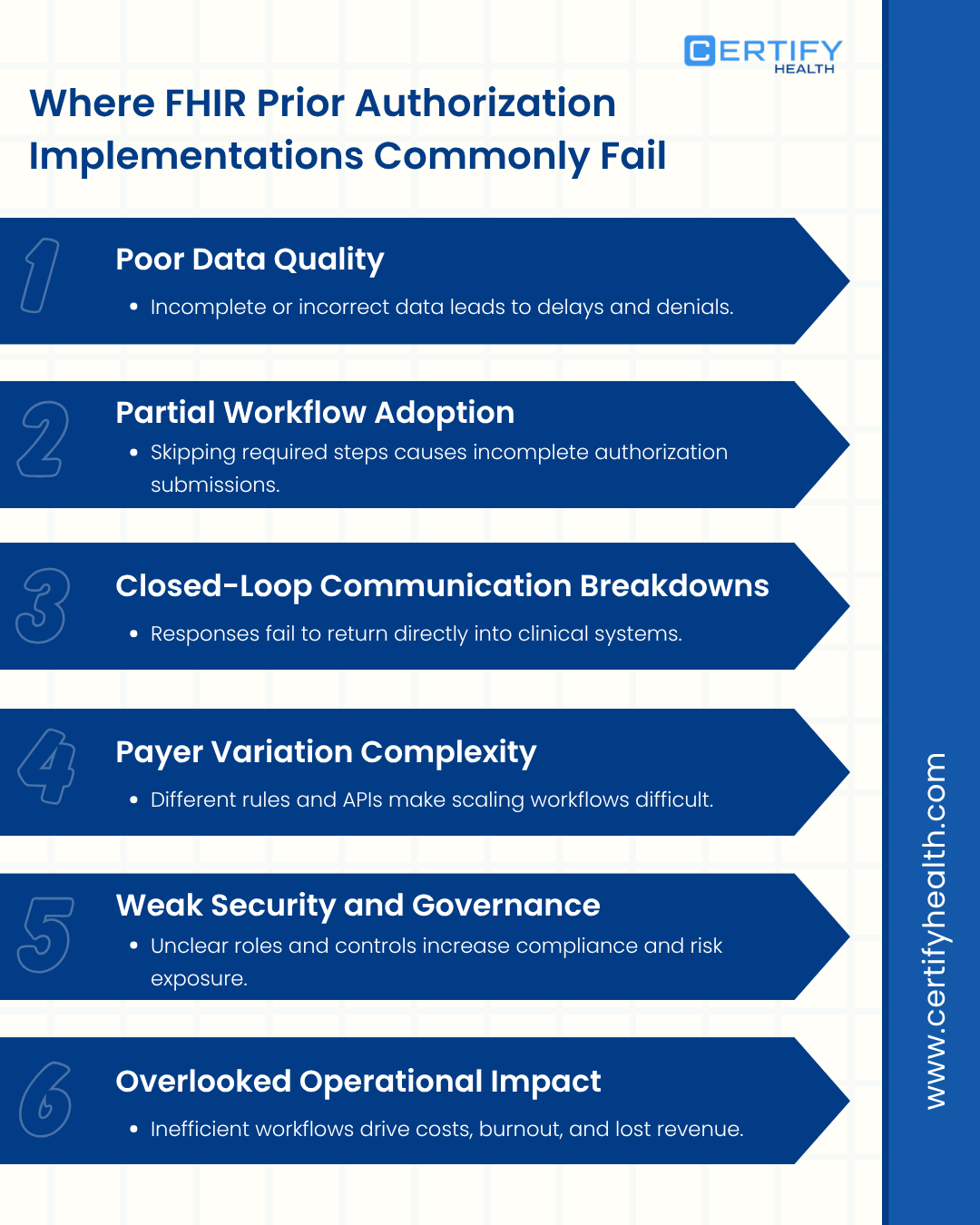
Where FHIR Prior Authorization Implementations Fail
Most failures happen in setup — not in the FHIR interoperability standard itself.
Bad Data Slows Everything Down
Incomplete charts. Wrong codes. Missing notes.
The FHIR API sends the request. The payer cannot use it.
Result: Delays, denials, and rework for staff.
Standards Are Skipped
Some systems skip key steps in DTR workflows. Teams do not see what documents are required.
Result: Incomplete submissions and more back-and-forth.
The Loop Never Closes
Requests go out. Approvals do not come back into the EHR. Staff check portals. They fax documents. The cycle repeats.
Result: Manual work returns. Productivity drops.
Every Payer Works Differently
Different payer APIs. Different rules. Different error messages.
Result: Scaling becomes slow and expensive.
Security and Governance Get Overlooked
Weak access controls. Poor workflow ownership. Technical fixes without clinical input.
Result: Risk goes up. Trust goes down.
The real cost shows up in operations:
- Longer turnaround times
- Higher denial rates
- More staff burnout
- Lost revenue
What CMS-0057-F Compliance Really Means for Your Organization

CMS-0057-F is not just an IT update. It changes how your organization works every day.
Decisions Must Happen Faster
- Standard requests: 7 days
- Urgent requests: 72 hours
No extensions. No delays. Slow workflows become compliance risks.
FHIR APIs Are Now Required
Systems must share data in real time. Patients, providers, and payers all connect through FHIR APIs. Old workarounds will not keep up.
Denials Must Be Clear
Generic responses are no longer allowed. Every denial needs a documented reason. Poor documentation leads to rework and audit risk.
Systems Must Speak the Same Language
Standard codes. Clean data. Connected workflows. Clinical and administrative systems must work together. Data gaps now show up as compliance gaps — a direct challenge to healthcare compliance and fhir interoperability.
Performance Will Be Measured and Reported
Approval times, denial rates, and patient access will become public metrics. Your operations directly affect your reputation and revenue.
Legacy Fixes Will Not Hold
Simple plug-ins on old systems break under pressure. Real-time FHIR data exchange needs modern infrastructure. Legacy system integration planning is essential — short-term patches create long-term risk.
Conclusion
FHIR APIs are becoming required infrastructure.
FHIR prior authorization will soon be measured, reported, and audited.
If your workflows are not tested end to end, you carry the risk: delays, denials, and missed timelines.
Run a readiness review now.
Book a Demo with CERTIFY Health — test these workflows in practice, not on paper.





















