Table of Contents
- End Revenue Loss: Healthcare data silos trap cash via claim denials healthcare and revenue leakage healthcare. A unified data model for healthcare unifies clinical EHR, billing, and patient engagement tool data for clean claims and fast payments.
- Stop Staff Burnout: Cut swivel chair work and reconciling data with HL7 FHIR integration and digital health infrastructure. Free staff for care, not chaos.
- Unlock Better Care: Beat healthcare interoperability challenges using enterprise data strategy and healthcare data unification. Get real-time population health insights and EHR integration.
At HIMSS 2026, leaders said it over and over. “We have the data. We can’t see everything in one view.“
That sums up data silos in healthcare today. Groups spend big on tools like EHRs and billing systems. They add patient engagement tool apps and analytics. But these systems don’t share information. This breaks things.
What happens?
- Lost revenue
- Slow care
- Tired staff
- Mad patients
These healthcare data silos cost more than most see.
What Are Data Silos in Healthcare?
Data silos in healthcare happen when systems hold data alone. They do not share well. Think of your healthcare IT system.
- A clinical EHR
- A specialty EMR
- Billing and RCM software
- A patient engagement tool
- Lab and imaging systems
Each grabs key facts. But no links mean trouble. You get many patient records. Not one true view.
Why Data Silos Persist in Healthcare

Healthcare interoperability challenges keep silos alive. Here is why.
- Old Systems: Many use legacy systems not built for interoperability in healthcare.
- Separate Buys: Teams pick tools on their own. No big plan. This causes splits.
- Vendor Traps: Some sellers use secret codes. This blocks EHR integration.
- Rules Get in Way: Laws guard data. But they slow healthcare data aggregation.
- No Common Way: Systems lack a unified data model. They do not match.
Where Data Silos Hit Hardest
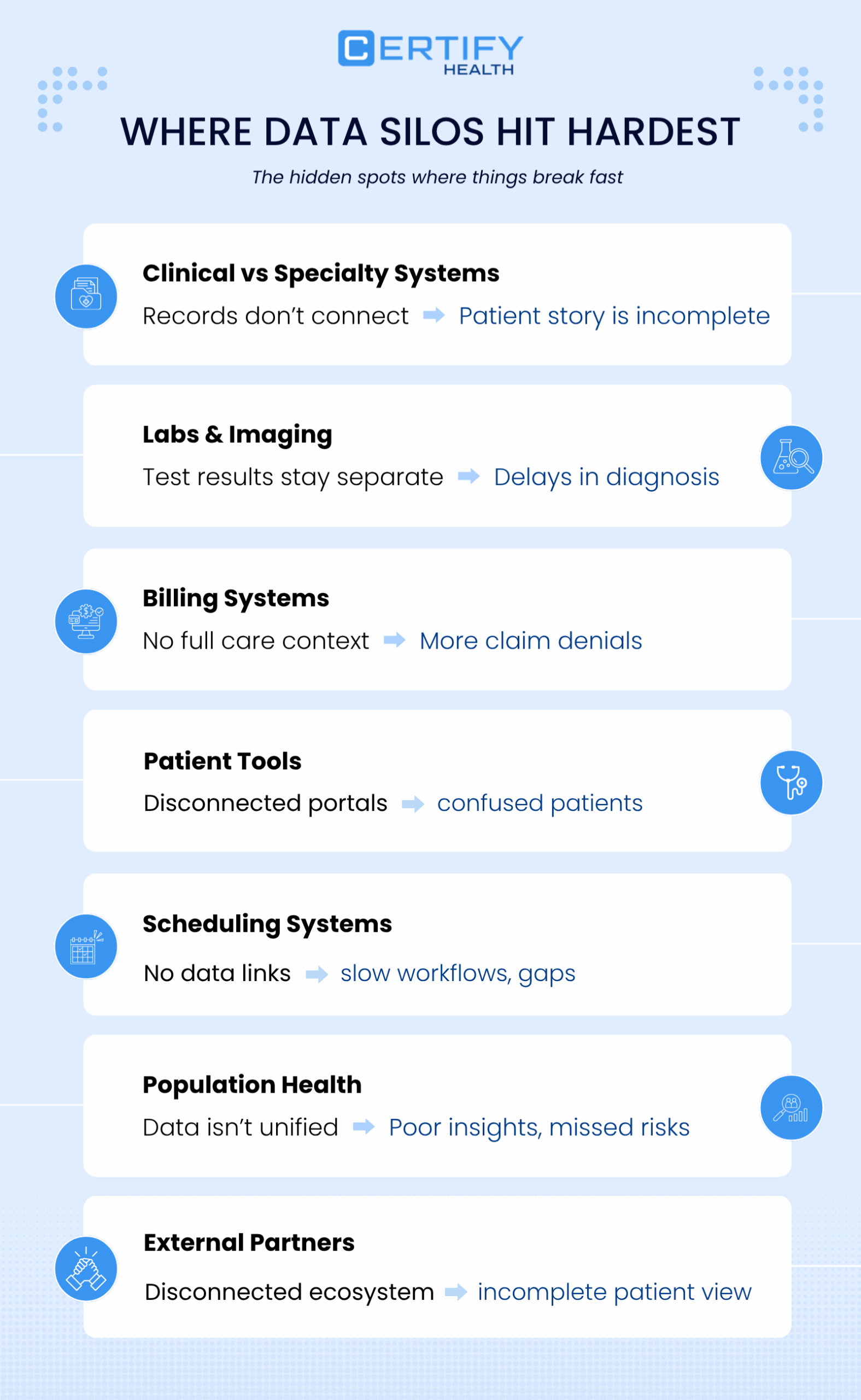
Silos hide in key spots. They hurt bad. Here are the top ones.
- Clinical vs. Specialty: Clinical EHR and specialty EMR stay apart. Patient stories break.
- Labs and Imaging: Test data sits alone. No fast views.
- Billing Split: Billing lacks full care facts. This drives claim denials healthcare.
- Patient Tools: Patient engagement tool skips links to care or bills. Messages clash.
- Scheduling: It ignores care or money data. Work slows.
- Population Health: No good healthcare data integration means weak population health views.
- Outside Groups: Drug stores, labs, and payers stay out. This adds healthcare interoperability challenges.
The Real Costs of Healthcare Data Silos
Silos do real harm. They hit care, money, and teams.
1. Patient Care Fails
Doctors miss facts from data silos in healthcare. They repeat tests. Diagnoses wait.
A study found that electronic records cannot be shared across systems. 32% of transferred patients experienced duplicate testing, and 20% of those tests were not clinically necessary.
2. Revenue Stays Trapped
Disconnected systems cause a lot of problems:
- Important details get missed
- Mistakes happen while coding bills
- More claims get denied
This also makes healthcare more expensive.
A study in Health Affairs found that about 1 out of every 4 dollars hospitals spend in the U.S. goes to administrative work, much of it caused by poor data sharing.
3. Staff Burnout Grows
Swivel chair work kills time. Doctors enter data twice. They chase records.
A study by American Hospital Association reveals that staff spend 49% of their time on EHR and desk work. It’s from healthcare data silos.
4. Choices Get Weak
Without healthcare data unification, leadership teams don’t get a clear picture of what’s happening.
- Reports may be wrong or incomplete
- Updates don’t happen instantly.
- It’s hard to track money and performance
Because of this, making good plans for the future becomes very difficult.
Why Healthcare Interoperability Challenges Linger
HL7 FHIR integration helps some. But problems stay. Formats do not match. Syncs skip real time. Links stay small. Healthcare interoperability solutions need more. A full digital health infrastructure is key.
The Fix: Unified Data Model for Healthcare
Stop silos with a unified data model for healthcare. It sets one way to hold and share data. No more moves between spots. It makes one true source.
It blends clinical EHR, ops, and money data. This brings healthcare data integration.
How It Helps:
- Easy EHR integration.
- Live data with HL7 FHIR integration.
- Less claim denials healthcare.
- Good patient talks via patient engagement tool.
- Strong population health facts.
Step-by-Step: Break Healthcare Data Silos
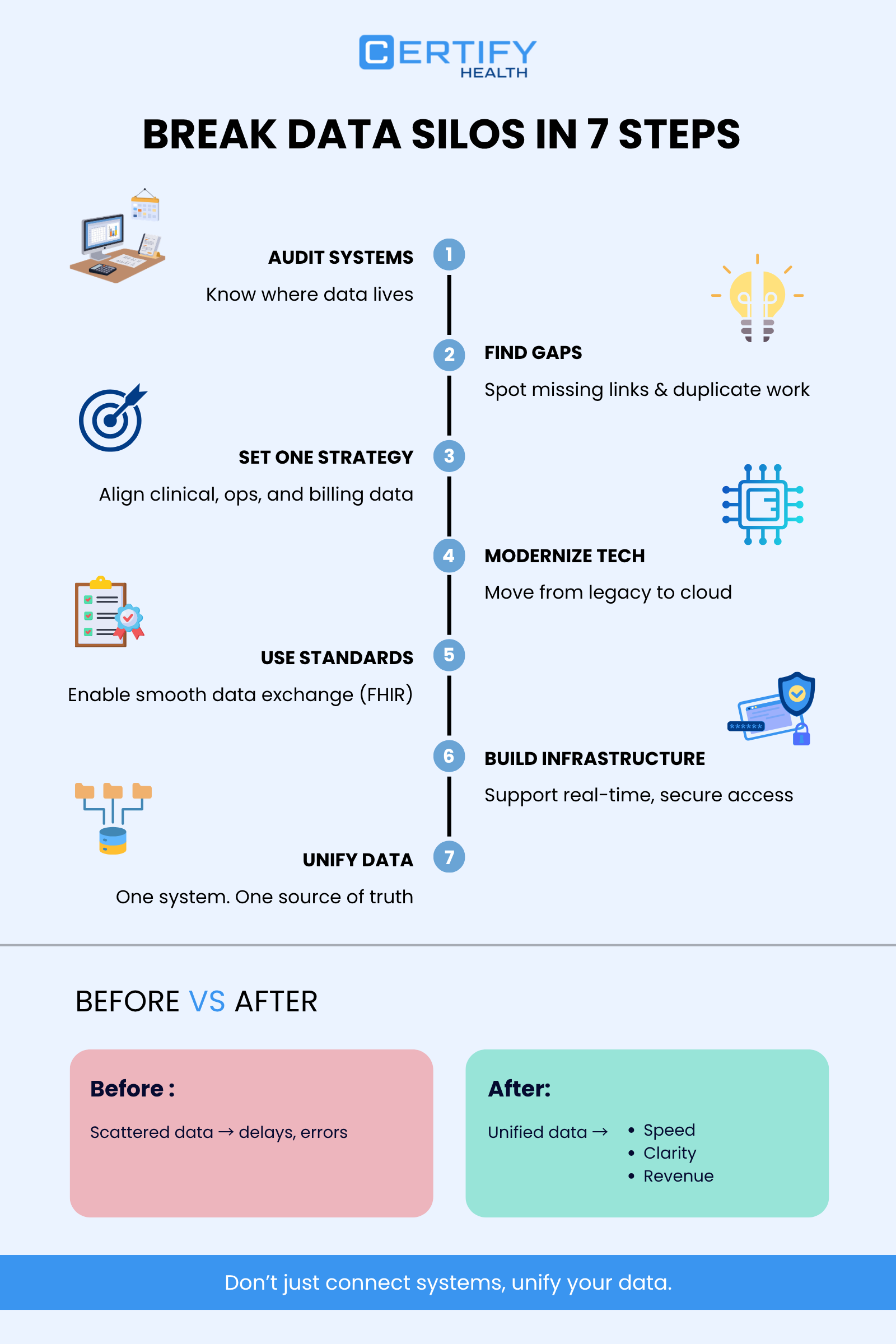
Fix needs plan and tech. Follow these steps.
Step 1: Check Systems
List all healthcare IT system parts. See what data each holds. Track where it goes. Spot stops.
Step 2: Find Gaps
Hunt for:
- Missing links
- Double data
- Hand work
Reconciling data is key here.
Step 3: Set Enterprise Data Strategy
Step 4: Do Healthcare Data Modernization
Update to healthcare data modernization. Drop old gear. Use cloud bases.
Step 5: Add Standards
Use HL7 FHIR integration for healthcare interoperability solutions.
Step 6: Build Digital Health Infrastructure
Step 7: Unify Data
Healthcare data unification joins systems as one. Not just links.
| Without Healthcare Data Unification | With Unified Data Model |
|---|---|
| Swivel chair work all day | Smooth flows |
| High claim denials healthcare | Clean bills, fast cash |
| Bad patient care | Full team work |
| Revenue leakage healthcare hides | Live facts shine |
The Bottom Line
Data silos in healthcare hurt more than IT. They trap cash and slow care.
They:
- Slow daily work
- Raise costs
- Cut care quality
Fix with enterprise data strategy. Add digital health infrastructure. At the center of it all is a unified data model for healthcare.
You have data. You lack joins. Fix that. Get better care. Happy teams. More money.
Want a free demo on how to fix your data silos in healthcare? Book one with CERTIFY Health.






















