Table of Contents
Introduction
Did you know that insurers deny about 20% of claims? That’s a big number. And many of those denials happen because of one simple mistake: not checking a patient’s insurance before the visit.
That’s what insurance eligibility verification is all about. It’s a quick check done before a patient comes in. It helps make sure their insurance is active and will cover the care they need.
When this step is skipped, it causes real problems. Bills get denied. Staff have to fix and redo work. Patients get surprise charges they didn’t expect. None of that is good.
Let’s break it down — what it is, how it works, and why it matters.
What Is Insurance Eligibility Verification?
Patient insurance eligibility verification means checking a patient’s insurance before their visit. It makes sure:
- Their plan is active on the day of the visit
- The service or treatment is covered
- The doctor or clinic is in-network
- The patient’s name, birthday, and ID match what’s on file
- Any needed approvals (prior authorizations) are in place
Don’t provide care and then find out the insurance won’t pay.
Medical insurance eligibility verification covers more than just a yes or no. It looks at co-pays, deductibles, coverage dates, and visit limits — all the details that affect billing.
Step-by-Step: How to Do a Healthcare Eligibility Check
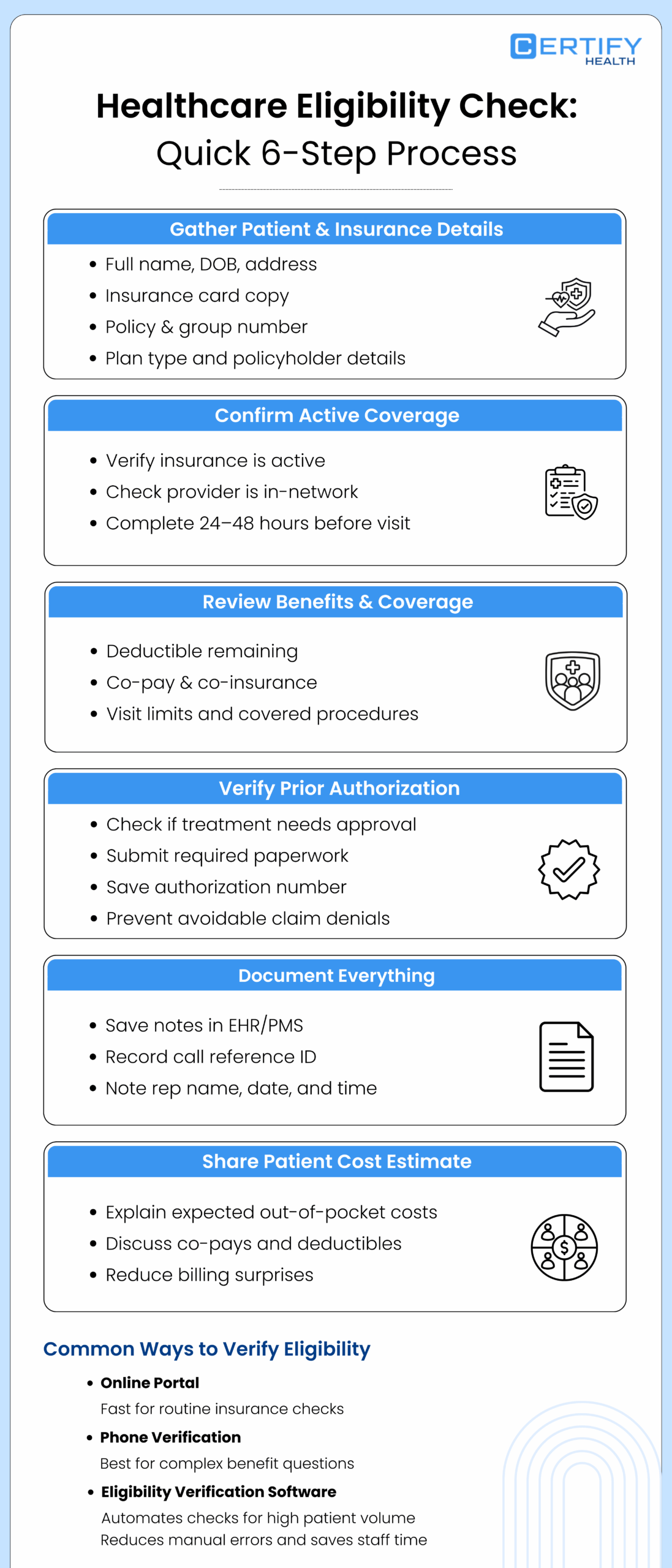
lways run a healthcare eligibility check 24 to 48 hours before the appointment. Here’s how it works:
Step 1: Collect Patient Info
Get the patient’s full name, date of birth, and address. Ask for their insurance card. Note the insurance company, policy number, group number, and plan type. Find out who holds the policy and when it started.
Step 2: Verify Coverage
Check the insurer’s website or your system, or call the insurer directly. Confirm the plan is active. Make sure the provider is in-network. Do this at least 48 hours before the visit.
Many practices also re-verify insurance before every visit, at the start of a new plan year, or whenever a patient reports coverage changes.
Step 3: Review Plan Benefits
Look at the full plan. Check the deductible balance, co-pay amount, co-insurance rate, and visit limits. Make sure the procedure code is covered.
Step 4: Check for Prior Authorizations
Some treatments need special approval before they’re done. This is called prior authorization. Getting this step right can help prevent up to 36% of denials. Check if it’s needed, get the approval number, and file the right paperwork.
Some payers also use terms like pre-certification or pre-determination, depending on the service and plan requirements.
Step 5: Record Everything
Save all notes in your EHR or practice management system. Write down the rep’s name, call ID, and date. This helps if there’s ever a billing dispute.
Step 6: Tell the Patient Their Costs
Let patients know what they’ll owe — co-pays, deductibles, or any charges not covered. When patients know their costs ahead of time, they’re less likely to be surprised or upset.
This step also supports compliance with the No Surprises Act and Good Faith Estimate requirements by helping patients understand expected costs before care is delivered.
Ways to Run Patient Eligibility Verification
Most electronic insurance checks use HIPAA-standard EDI 270/271 transactions.
The provider sends a 270 eligibility request to the insurance payer.
The payer then sends back a 271 response with details like:
- Insurance coverage
- Deductibles
- Co-pays
- Plan status
Medicare uses CMS’s HETS (HIPAA Eligibility Transaction System) for eligibility verification.
Medicaid eligibility rules can vary by state and by payer network.
Behind the scenes, that’s the protocol most systems use. From the staff side, there are three practical ways to run a check:
- Online portal: Fast and easy for simple checks.
- Phone call: Slower, but good for complex cases.
- Insurance eligibility verification software: The best option for busy offices. It handles many patients at once with fewer errors.
Many healthcare organizations connect eligibility verification with their EHR, scheduling, and practice management systems to reduce duplicate data entry and speed up front-desk workflows.
Common Problems in Insurance Eligibility Verification

Even when teams try hard, mistakes happen. Here are the most common insurance eligibility mistakes:
- Wrong Patient Info: A typo in a name or birthday can cause a mismatch. Insurance eligibility verification software helps by capturing data accurately and reducing human error.
- Insurance That Changed or Ended: People switch jobs. Dependents age out of plans. Policies lapse. That’s why it’s so important to check close to the visit date — not weeks before. If no active coverage is found, staff may transition the patient to self-pay workflows or offer payment plans before the visit.
- Complex Plan Rules: Every plan has different rules about what’s covered, what’s not, and what needs pre-approval. These are hard to track by hand.
- Slow Manual Checks: Calling insurers takes a long time. When offices are busy, checks fall behind. Automated insurance verification software speeds this up.
- Missed Prior Authorizations: If a service needs prior approval and no one gets it, the claim gets denied — even after care is already provided.
- Multiple Insurance Plans: Some patients have more than one insurance plan. Staff must follow coordination of benefits (COB) rules to know which insurance should be billed first. If they bill the wrong insurance first, the claim may be delayed, denied, or sent back to be fixed.
- Staff Turnover: When experienced staff leave, new staff make more errors. This is when verification mistakes spike.
- Talking to Patients About Costs: Discussing money can be uncomfortable. Insurance verification software makes it easier by letting staff share cost details through text, email, or a patient portal.
What Happens When Eligibility Verification Fails?
When insurance eligibility is not verified correctly, it can cause problems for both billing and patient care.
- Claims may be denied, rejected, or delayed
- Payments slow down and revenue is affected
- Some services may not be paid at all if errors cannot be fixed
- Staff spend more time correcting claims and calling payers
- Missing prior authorization can lead to automatic denials
- Patients may receive unexpected bills
- Care can be delayed in some cases
- Front desk teams may collect incorrect payments
Fixing eligibility issues early helps avoid billing problems and keeps care moving smoothly.
Why Patient Eligibility Verification Matters
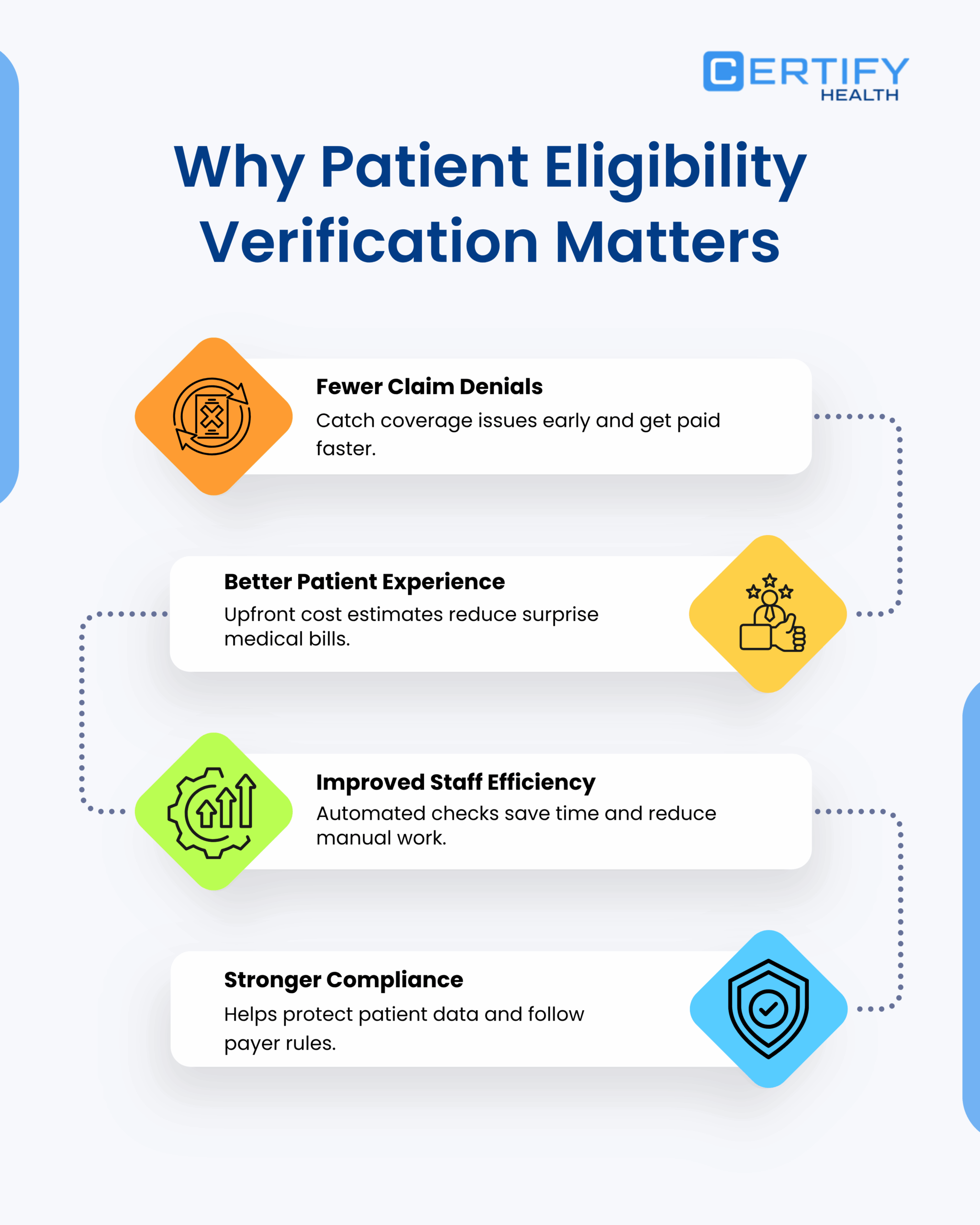
Strong eligibility workflows also improve key revenue cycle metrics like clean claim rate, first-pass claim acceptance, denial rate, and days in accounts receivable (A/R).
- Fewer Denials, More Revenue: When you run patient eligibility verification before every visit, you catch problems early. Fewer denials mean less time spent fixing and resubmitting claims. That means faster payment.
- Better Patient Experience: No one wants a surprise bill. When patients know their costs upfront, they trust you more and pay on time.
- More Efficient Staff: Real-time insurance eligibility checks remove the need for long calls and manual typing. Staff can spend their time on more important tasks.
- Staying Compliant: Insurance eligibility verification software helps protect patient data and follow payer rules. This lowers the risk of fraud, audits, and penalties.
How Insurance Eligibility Verification Software Helps
Manual checks are slow and easy to mess up. CERTIFY Health’s unified medical practice software makes this process simple with smart, automated tools built into one system.
With our insurance eligibility verification software, staff can:
- Run real time insurance eligibility verification before the patient even walks in
- See full coverage details — deductibles, co-pays, visit limits, and approvals — all in one place
- Scan insurance cards to reduce typing errors
- Verify insurance 48 hours before the visit or at check-in via kiosk or mobile
- Connect directly with scheduling and billing so there’s no switching between apps
What offices gain:
- Fewer denied claims
- Faster payments
- Less manual work for staff
- Better experience for patients — no surprise bills
One CERTIFY Health client saw a real improvement after switching to automated insurance eligibility verification. Billing delays went down. Admin rework dropped. The front desk ran smoother.
Want to see it yourself?
Wrap-Up
Insurance eligibility verification is not just a front-desk task. It protects your revenue and your patients.
When you run a healthcare eligibility check 24 to 48 hours before every visit, you catch problems early. Claims get paid faster. Staff spend less time on rework. Patients know what to expect.
Small errors — a missed approval, wrong plan, bad coverage detail — can lead to denied claims and billing delays. But they’re easy to prevent when you verify early.
If your team is still doing this by hand, it may be time to switch. Healthcare workflow automation through tools like CERTIFY Health can cut errors, save time, and make billing smoother for everyone.
Check early. Check right. Tell patients what they owe. That simple habit makes a big difference.





















