Table of Contents
Dermatology practices operate under one of the most demanding operational models in outpatient care.
High patient throughput, short visit durations, complex procedure documentation, and heavy insurance interaction converge into a system where manual workflows directly cap revenue.
Administrative work accounts for over 30% of physician time, with prior authorization, eligibility checks, documentation, and billing representing the largest share of non-clinical labor.
Automation in dermatology is not about convenience. It is about protecting revenue per visit, reducing administrative overhead, and preventing revenue loss before it occurs.
Why Dermatology Is One of the Most Automation-Dependent Specialties
Dermatology combines high visit volume with high documentation and billing complexity. That combination is rare and unforgiving when workflows are manual.
High Patient Throughput Creates Hidden Operational Drag
Dermatology visits are short, but the operational steps around them are not. A national study published in JAMA Dermatology found dermatology clinic no-show rates ranging from 7.8% to 31.0%, depending on reminder systems and scheduling practices. Each missed appointment represents unused clinical capacity and lost revenue.
High daily appointment volume amplifies small inefficiencies. Manual appointment scheduling, plans to automate dermatology scheduling, manual reconciliation, and manual intake errors scale faster than revenue.
The Unique Revenue Mix in Dermatology
Dermatology revenue spans:
- Medical dermatology billed through insurance
- Surgical dermatology requiring precise CPT documentation
- Cosmetic and self-pay services with direct patient payments
This mixed revenue model increases automation dependency, especially around eligibility checks, charge capture, and patient payments. Practices relying on manual processes experience higher administrative overhead and greater revenue variability.
The Profit Leaks Most Dermatology Practices Don’t Track
Administrative Overhead That Scales Faster Than Revenue
Administrative overhead is not abstract. U.S. healthcare spending analysis shows administrative costs consuming 17% to 25% of total healthcare expenditures, far higher than peer nations.
In dermatology, prior authorization is a dominant driver. A U.S. academic dermatology department measured 170 staff hours per month dedicated solely to prior authorizations, with some cases taking up to 31 business days to resolve.
Manual intake, repetitive eligibility checks, and follow-ups inflate overhead without increasing visit volume.
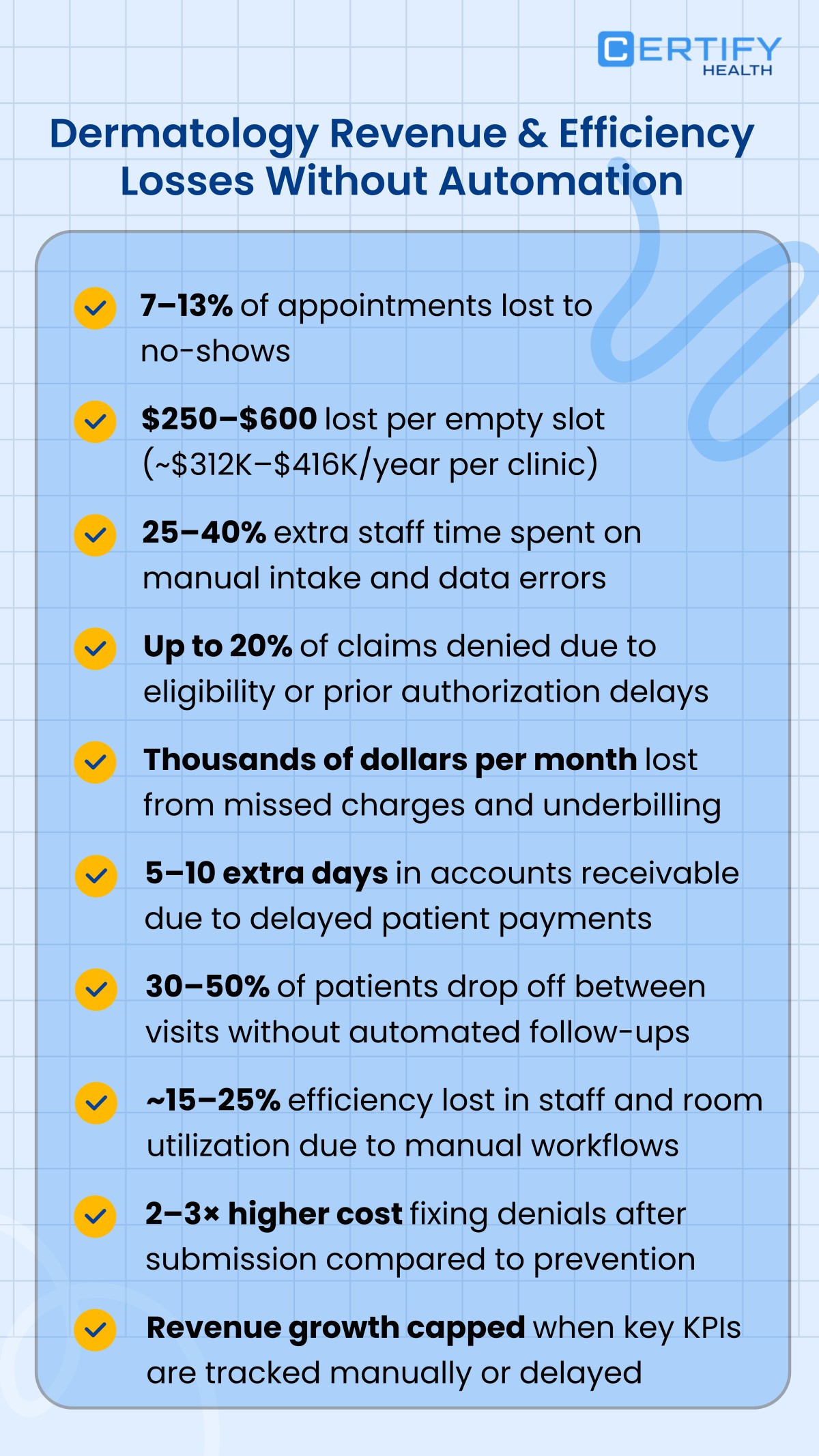

Revenue Lost to No-Shows, Underbilling, and Denials
Data shows claim denials remain widespread. Analysis of in-network claims reveals denial rates approaching 19%, with incomplete information and eligibility errors among the top causes.
In dermatology, missed procedure documentation and delayed charge capture further reduce realized revenue per visit.
Why Point Automation Tools Fail to Improve Dermatology Margins
Siloed Systems Increase Rework Instead of Reducing It
Scheduling systems that do not feed intake. Intake platforms that do not upgrade dermatology billing performance. Billing systems disconnected from clinical documentation.
This fragmentation forces manual reconciliation and duplicate data entry, which federal workflow studies consistently identify as a leading source of administrative waste.
Automation Without Interoperability Still Requires Staff Bandwidth
When systems do not share structured data, staff become the integration layer. Manual handoffs increase error rates and negate automation gains.
End-to-end automation is the only model that reduces labor while improving accuracy.
The 10 Dermatology Processes You Must Automate to Maximize Profits
1. Appointment Scheduling and Demand Routing
Scheduling directly affects utilization. A national dermatology access study showed appointment acceptance rates exceeding 94% for privately insured patients, but much lower when scheduling constraints exist.
What automation changes operationally:
- Visit-type logic separates new vs returning patients
- Medical, surgical, and cosmetic visits are routed into correct time blocks
- Demand routing reduces idle provider time and overbooking conflicts
2. Digital Patient Intake and Pre-Visit Data Collection
Manual intake errors propagate downstream. Inaccurate demographics and insurance data are leading causes of claim rework.
Automated intake eliminates redundant questions, improves completion rates, and feeds structured data directly into eligibility and billing workflows.
This reduces downstream denials and shortens check-in time.

3. Insurance Eligibility and Coverage Validation
Eligibility errors are a major denial driver. Federal analyses show eligibility mismatches among the most common causes of claim rejection across outpatient care. This also encompasses end-to-end rcm for dermatology practices as they are form a integrated ecosystem.
Automation impact:
- Real-time eligibility checks before visits
- Patient corrections triggered pre-arrival
- Fewer write-offs and surprise balances
4. Prior Authorization for High-Value Dermatology Procedures
Prior authorization is one of the most burdensome workflows in dermatology. A U.S. survey found staff spending over 3 hours per day on authorizations, with 24% taking more than one week.
Automation specifics:
- CPT- and diagnosis-based authorization triggers
- Automated submissions and follow-ups
- Faster treatment starts and fewer abandoned procedures
5. Front-Desk Check-In and Visit Readiness
Manual check-in increases wait times and staff workload.
Manual intake heavily contributes to administrative burden as U.S. providers collectively spend about 25% of total healthcare spending on administrative activities including intake, insurance checks, eligibility verification, billing, and claims processes.
Manual demographic entry is tied to downstream issues (e.g., denials and rework). These intake errors contribute to the high administrative costs (e.g., improper payments partly due to documentation/eligibility lapses).
Pre-visit automation ensures intake, eligibility, and payments are complete before arrival, reducing touch time per patient.
6. Procedure Documentation and Charge Capture
Incomplete documentation leads to underbilling.
Insufficient documentation accounts for most improper Medicare payments.
In FY2024, about 79% of Medicaid improper payments were due to insufficient documentation, indicating a direct link between documentation quality and payment accuracy.
Charge capture automation maps procedures directly to billing codes, reducing under coding and missed services.
7. Claims Submission and Denial Prevention
Federal data shows nearly 1 in 5 claims face denial or rejection. Automation that uses validated intake and eligibility data significantly improves clean claim rates.
Tools like CERTIFY Health help achieve dermatology denial rate benchmarks of 95+. Clean claim rate is frequently used in federal and industry practice benchmarks to represent timely and accurate claims submission.
8. Patient Payments and Financial Responsibility Communication
Automated cost estimates and payment workflows reduce disputes and accelerate collections.
Administrative steps like documentation and verification directly impact claims integrity and cash flow — up to tens of billions of dollars annually in improper payments tied to insufficient documentation and administrative errors.
Clear financial responsibility communication improves payment timing and patient satisfaction.
9. Referral, Follow-Up, and Recall Management
Missed follow-ups contribute to revenue leakage. Automated recall systems improve retention and continuity of care, particularly chronic dermatologic conditions.
Improving automated outreach and follow-up is associated in practice data with improved retention and continued care, particularly for chronic conditions, and reduces revenue leakage tied to gaps in care delivery and billing capture.
10. Operational and Financial Performance Tracking
Practices that track KPIs outperform peers. Key metrics include:
- Revenue per visit
- No-show rate
- Denial rate
- Front-desk cost per patient
Automation enables real-time visibility and continuous optimization.
How CERTIFY Health Enables End-to-End Dermatology Automation
CERTIFY Health unifies:
- Appointment scheduling
- Digital intake
- Eligibility checks
- Prior authorization
- Charge capture
- Billing and analytics
No point solutions. No data silos. One operational spine.
Built for high-volume, multi-location dermatology practices, CERTIFY Health is EHR-agnostic, dermatologist patient revenue platform and designed to scale without adding staff.
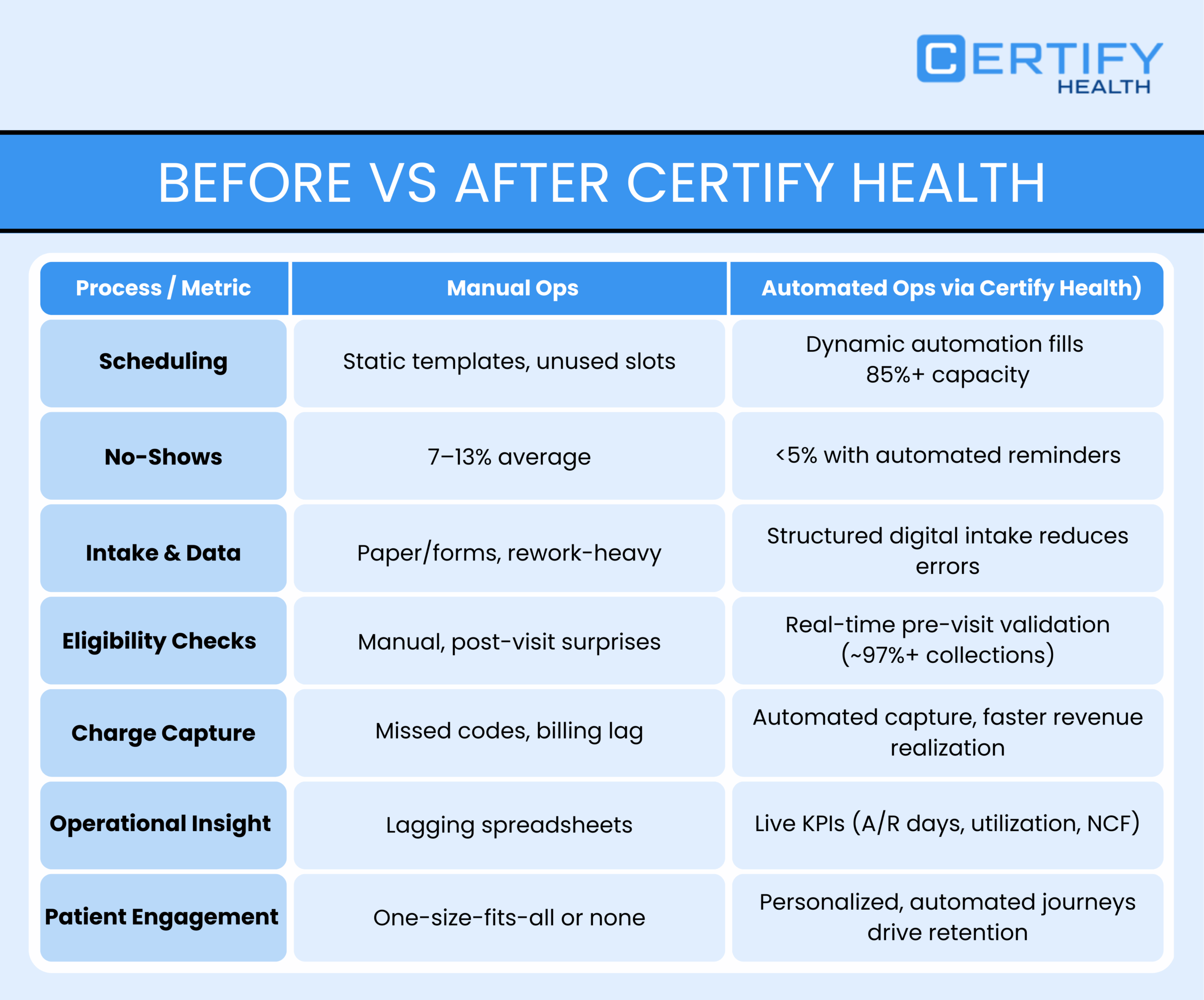
Final Takeaway: Profitability in Dermatology Is an Automation Problem
Federal and peer-reviewed research is clear. Manual workflows increase overhead, inflate denial rates, and cap growth.
The standout tool for this is CERTIFY Health, because it addresses automation as a system, not a feature. It is dermatology revenue intelligence software. By connecting patient access, intake, eligibility, billing, and analytics into a single workflow, CERTIFY Health eliminates leakage and enhances dermatology revenue cycle management at every stage.
Next Step
Assess your dermatology automation readiness. Schedule a CERTIFY Health demo and identify the exact workflows limiting your revenue today.
Frequently Asked Questions
What is revenue cycle management for dermatology practices?
Revenue cycle management (RCM) in dermatology refers to the complete process of capturing patient information, verifying insurance, submitting claims, collecting payments, and managing accounts receivable. Efficient RCM ensures dermatology practices receive timely reimbursement while minimizing billing errors and administrative delays.
Why is patient revenue cycle management important for dermatology clinics?
Dermatology practices often handle high patient volumes, cosmetic procedures, and insurance variations. Strong patient revenue cycle management improves claim accuracy, speeds up payment collection, reduces denials, and ensures a smoother financial workflow for the practice.
How can dermatology practices improve their revenue cycle management?
Practices can improve RCM by automating patient intake, verifying insurance eligibility in advance, using digital payment tools, and monitoring claim performance through analytics dashboards. Automation reduces manual errors and accelerates collections.
How do dermatology patient intake solutions help streamline operations?
A digital patient intake solution allows patients to complete forms online, verify insurance, and update medical history before their appointment. This reduces front-desk paperwork, speeds up check-in, and ensures accurate information flows directly into billing and clinical systems.
How should practices compare dermatology revenue cycle management solutions?
When comparing RCM solutions, dermatology practices should evaluate automation capabilities, integration with EHR systems, patient communication tools, analytics dashboards, and payment collection features. Solutions that unify intake, scheduling, and billing workflows typically deliver the best results.
How can CERTIFY Health support dermatology patient intake and revenue cycle workflows?
CERTIFY Health helps dermatology practices streamline patient intake, automate insurance verification, simplify scheduling, and enable digital payment options. These connected workflows reduce administrative burden while improving revenue collection and patient experience.






















