Table of Contents
- Interoperability barriers, such as legacy systems, inconsistent data, and regulatory complexity, slow care coordination, and increase administrative burden.
- Standards like HL7 FHIR, combined with strong data governance and integration platforms, enable secure real-time data exchange.
- Healthcare organizations that invest in interoperable platforms see improvements in operational efficiency, revenue cycle performance, and patient experience.
- Modern healthcare interoperability platforms help unify EHRs, billing systems, and patient engagement tools into a single integrated ecosystem.
Healthcare organizations generate massive volumes of clinical data, but much of it remains trapped in disconnected systems. A national study analyzing 2,420 U.S. hospitals found that while 71% of hospitals can electronically access patient information from external providers, only 42% routinely use that data in clinical care due to persistent interoperability barriers.
These gaps create fragmented care experiences. When EHRs, billing systems, labs, and patient portals fail to communicate effectively, clinicians struggle to access complete patient histories, leading to delayed decisions, duplicated tests, and inefficient workflows.
An integrated health care system addresses this fragmentation by enabling secure, real-time data exchange across clinical and administrative platforms, giving providers a unified view of patient information while improving operational coordination.
Mastering EHR interoperability is the foundation of truly integrated healthcare. It breaks down data silos, improves patient outcomes, strengthens compliance, and supports value-based care.
In this post, we examine the most pressing interoperability challenges and the evidence-based strategies health systems can use to overcome them.
The Hidden Costs of Poor Interoperability in Healthcare
Poor interoperability does more than slow data exchange; it creates measurable operational and financial losses across the healthcare system.
Fragmented health IT systems force clinicians to search across multiple platforms to assemble a complete patient record. Studies show physicians spend nearly 50 minutes per day reconciling information across different EHR systems, contributing to an estimated $15.4 billion in annual productivity losses.
Data silos also drive unnecessary clinical spending. When prior records or test results are unavailable, providers often repeat diagnostics. Analysts estimate that lack of interoperability costs the U.S. healthcare system more than $30 billion annually through duplicate tests, administrative overhead, and delayed treatment decisions.
Beyond cost and efficiency, these gaps affect care quality. Missing data can lead to treatment delays, repeated procedures, and incomplete patient histories.
Quick Comparison of Siloed vs Integrated Healthcare System
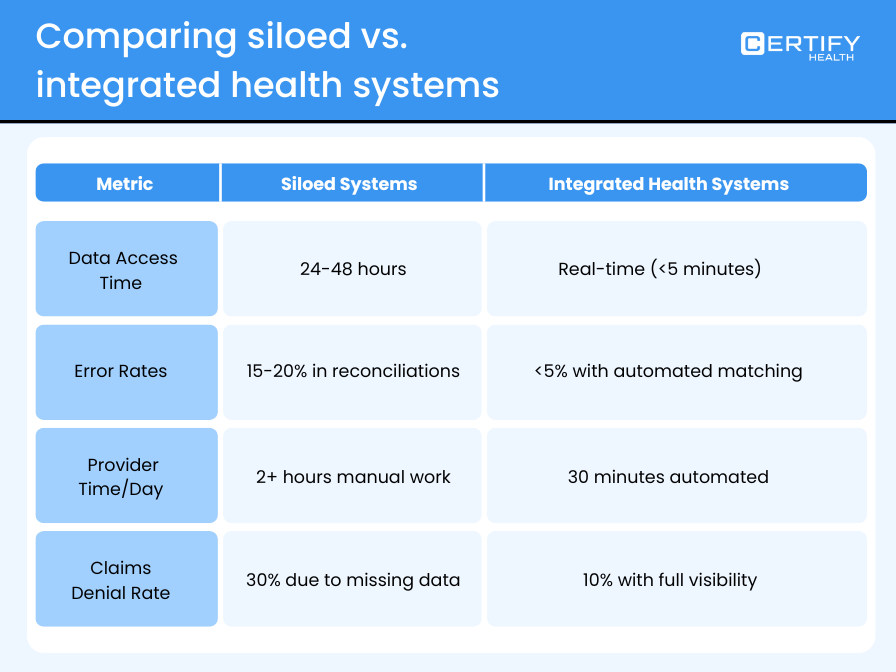
Key Barriers to Integrated Health Care Systems
While challenges exist, focusing on healthcare interoperability solutions helps practices move forward. Here are the key barriers to an integrated health care system, with eyes on fixes.
1. Legacy System Incompatibility
Many legacy systems lack modern APIs, making it difficult to exchange data with newer platforms. Proprietary formats add friction, turning simple data shares into headaches. Over years, point-to-point links build a tangled web that’s hard to untangle or expand.
Solution:
Start with healthcare data integration solutions that add an integration layer to translate legacy formats into modern standards like HL7 or FHIR, allowing older systems to exchange data without replacing the entire infrastructure.
2. Data Quality and Inconsistency
Healthcare data silos breed mismatches, like different patient IDs across platforms, leading to duplicates and blind spots. Manual entry worsens it; slowing processes in what should be a seamless integrated health care system.
Solution:
Implement EHR interoperability solutions with master patient indexing and automated validation rules to standardize patient identifiers and eliminate duplicate records across systems.
3. High Costs and Resource Constraints
Integration feels like a big upfront spend, with consulting fees stacking up before results show. Maintenance drains budgets further, especially without in-house skills for integrated medical systems.
Solution:
Adopt integrated systems solutions with modular integration platforms that allow practices to connect systems gradually, reducing upfront investment and spreading costs across phased deployments.
4. Security and Compliance Risks
Linking systems opens more doors to threats, and keeping data compliant across integrated health systems gets tricky with varying vendor updates.
Solution:
Using healthcare interoperability platforms that enforce encryption, role-based access, audit trails, and continuous compliance monitoring across connected systems.
5. Organizational and Cultural Barriers
Staff stick to old habits, managers question spends on integrated medical systems software, and departments pull in different directions.
Solution:
Interoperability challenges and solutions require buy-in from leadership. Create cross-department governance teams and provide workflow training so staff understand how integrated systems improve daily operations.
6. Scalability and Future-Proofing
Rigid setups choke under growth, and vendor choices lock practices into dead ends, blocking a flexible integrated health care system.
Solution:
Build integrations on standards-based APIs and cloud-ready architecture, so new systems, partners, or locations can be added without rebuilding connections.
7. Performance Degradation
Heavy integrations tax networks, causing lags when real-time needs meet slow batch processes, undermining EHR interoperability.
Solution:
Use event-driven data exchange and real-time APIs instead of batch processing to keep systems synchronized without slowing performance.
Want a checklist to evaluate your integrated health care system? Grab our free roadmap template now.
Proven Strategies to Achieve EHR Interoperability in Value-Based Care
The real value lies in action. These healthcare interoperability solutions turn interoperability challenges and solutions into strengths for your integrated health care system. Practices already aware of healthcare interoperability challenges can jump straight to implementation.
1. Adopt Standardized Data Formats and Protocols
Switch to HL7 FHIR for API-based links that allow EHR interoperability solutions to exchange data consistently across integrated medical systems. Pair it with standardized coding systems such as SNOMED CT and ICD-10 to align clinical and billing terminology across platforms. Open APIs reduce proprietary integration barriers and enable more seamless data exchange within an integrated health care system.
This foundation supports the importance of EHR interoperability in value-based care enablement platforms, where timely data sharing helps improve care coordination and supports accurate reimbursement.
CERTIFY Health supports interoperability standards such as HL7 FHIR, along with widely used clinical and billing code systems like SNOMED CT and ICD-10, helping healthcare organizations connect EHRs and other platforms more efficiently.
2. Implement Strategic Data Governance and Quality
Build a master patient index to match records accurately, wiping out healthcare data silos in your integrated health care system. Add validation tools to catch errors during entry or transfer. Set governance rules for access and security, ensuring HIPAA holds across integrated health systems.
3. Utilize Advanced Technology Solutions
Join Health Information Exchanges for broad data sharing beyond your walls. Cloud platforms scale storage and access for healthcare data integration solutions in multi-site setups. Automation handles mapping messy data and pulls insights from notes, boosting EHR interoperability efficiency.
4. Enhance Workflow Integration and User Experience
Embed data right into daily tools, skipping extra logins for clinicians. SMART on FHIR apps slot in features like calculators directly into EHRs. Unified patient portals give families one view of records from all providers, strengthening the integrated health care system.
5. Focus on Organizational and Security Strategies
Use role-based controls to limit access during flows. API-led designs reuse connections, cutting custom work. Craft a phased plan tying integrations to goals like fewer readmissions, aligning your full integrated health care system with value-based care.
Real-World Wins: Integrated Systems in Action
Healthcare organizations investing in an integrated health care system quickly see measurable improvements across operations, finances, and care coordination. When interoperability in healthcare is implemented effectively, data moves seamlessly across EHRs, billing platforms, and patient engagement tools, unlocking tangible results.
Operational Wins
Integrated workflows reduce manual work and improve data accessibility. With strong EHR interoperability, clinicians and staff can access patient records instantly across departments. This eliminates duplicate data entry, reduces redundant tests, and allows teams to coordinate care more efficiently across integrated health systems.
Financial Wins
Financial performance improves when clinical and billing systems communicate in real time. Organizations using modern healthcare interoperability platforms report faster claim submissions, fewer documentation gaps, and lower denial rates. By aligning clinical documentation with billing processes, integrated systems solutions help accelerate reimbursements and improve revenue cycle performance.
Team and Care Coordination Wins
Perhaps the most immediate impact is on the care team. When providers share a unified patient record across integrated medical systems, collaboration becomes easier between specialists, primary care providers, and administrative staff. This improves decision-making, reduces clinician frustration, and strengthens patient experiences
Ready to see how interoperability can transform your operations?
Book a Demo with us and explore how CERTIFY Health helps organizations implement practical healthcare interoperability solutions for value-based care.
Building Your Roadmap to a Truly Integrated Health Care System
Turn plans into progress with this decision-stage checklist for your integrated health care system:
- Audit your stack for EHR interoperability weak spots, focusing on healthcare data silos.
- Test integrated systems solutions with FHIR-based pilots in one department.
- Partner with experts for scalable healthcare data integration solutions that fit value-based shifts.
Conclusion
Healthcare organizations don’t lack data; they struggle with disconnected systems that trap critical information across EHRs, billing tools, and patient platforms. When interoperability gaps persist, teams rely on manual workarounds, workflows slow down, and errors impact both care coordination and revenue cycle performance.
The operational cost is significant: delayed decisions, administrative burden, fragmented patient experiences, and missed opportunities for value-based care.
A modern healthcare interoperability platform solves this by connecting systems through standards-based integrations, enabling secure, real-time data exchange and unified patient records.
Platforms like CERTIFY Health help organizations eliminate data silos, streamline operations, and build a truly integrated health care system.






















